In this month’s Prosthodontips, Josh Sharpling and Zohaib Ali cover the thorny subject of occlusion and whether to restore by canine guidance or group function.
In this month’s Prosthodontips, Josh Sharpling and Zohaib Ali cover the thorny subject of occlusion and whether to restore by canine guidance or group function.
In the last columns, we have discussed treatment options for rehabilitating patients with tooth wear. Today we are going to very lightly step into a huge dental topic, which can cause big arguments and huge controversy!
We are going to discuss…occlusion.
Specifically, we are going to discuss whether to restore somebody into canine guidance or group function.
The elephant in the room with any topic related to occlusion is temporomandibular disorders (TMD). Several systematic reviews (Manfredini Lombardo and Siciliani, 2017; Abduo, Tennant and McGeachie, 2013) show there is no relationship between lateral occlusal scheme and TMD.
Kahn et al (1999) also shows there is no relationship between TMD and non-working side interferences. This point may already be the start of controversy for some; however, we hope the evidence will keep a lid on that can of worms for now.
Now that we have put TMD to one side, we will focus on the decision-making process when designing lateral guidance. Occasions where you may need to consider lateral guidance design include:
- Treating tooth wear (when conforming or reorganising)
- Broken restorations/teeth fractures
- Aesthetic rehabilitation
- When restoring a tooth/teeth that are currently involved in lateral guidance
- Implant restorations
- Complete dentures.
Canine guidance
Canine guidance is often looked upon as the ideal lateral guidance scheme. This is because canine guidance will produce immediate disclusion of posterior teeth in excursions (one aspect of what is known as a ‘mutually protected occlusion’).
Disclusion of the posterior teeth will reduce lateral forces on these teeth, reducing the chance of fracturing teeth/restorations.
A heavily restored posterior dentition, with a history of fractures, may benefit from converting to canine guidance. This will also limit lateral forces on the weakened posterior teeth.
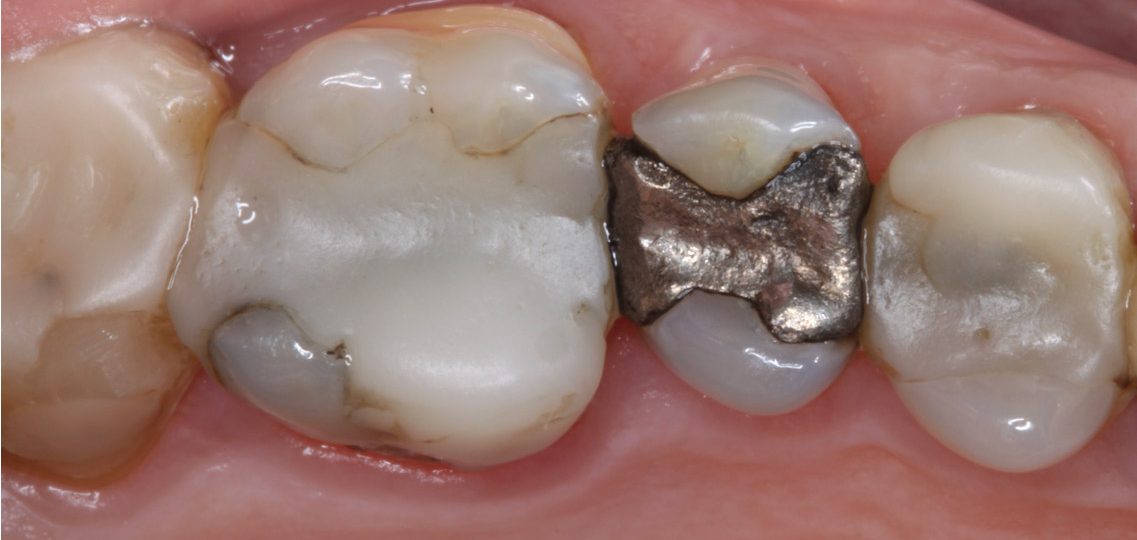
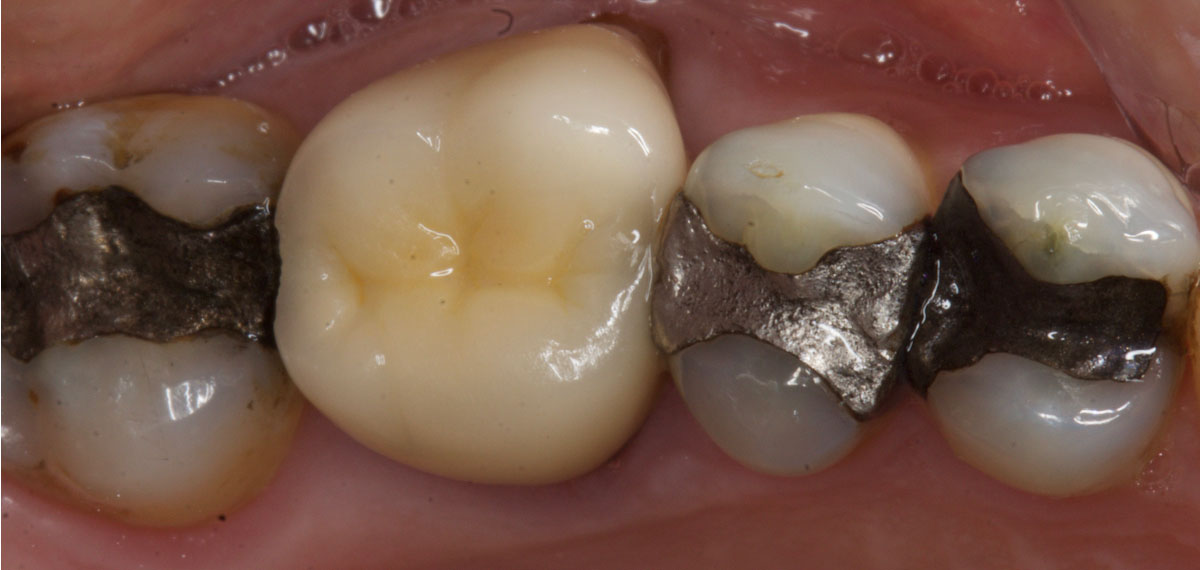
Patients in both of the photos below have heavily restored posterior dentitions. You could also make an argument that several cuspal coverage restorations are indicated.
However, if the patient did not consent to this, but wished to limit the risk of future fractures, then restoring the canines and ensuring canine guidance (for instance by canine rises in composite) would do this.
The occlusal reasoning behind canine guidance is shown above. However, there is also a practical argument; it is relatively easy to design an occlusion with canine guidance.
Steep inclines on the palatal surfaces of upper canines (either on models in a dental lab/CAD software, or clinically) will almost always produce canine guidance.
Producing accurate group function is much more difficult. It requires accurate records on a semi-adjustable articulator. Often alongside significant clinical adjustment.
Group function
So far, we’ve said that canine guidance is easier to produce, reduces posterior lateral forces, and has the same outcomes in TMD as group function. So why would you ever want group function?
There are a few specific reasons:
- Heavily restored canine
- A root-treated canine with a post may not be suitable for guidance. Therefore it is better to share guidance amongst other posterior teeth
- An implant replacing a canine may not be suitable for guidance
- Multiple unit implant restorations
- In full arch restorations, or restorations involving the canines and premolars group function and shallow guidance is beneficial to share occlusal forces (Gross, 2008)
- Class III incisal relationship
- In patients with a class III incisal relationship, it is very difficult, if not impossible, to design an occlusal scheme with canine guidance
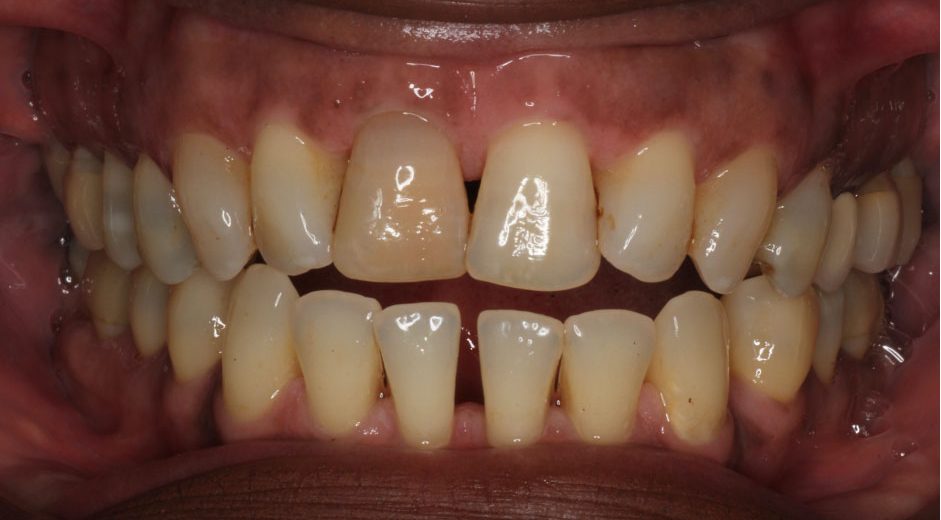
- Anterior open bites
- Similar to those with class III relationships. It is impossible to design a canine-guided occlusal scheme in these patients (see Figure 3)
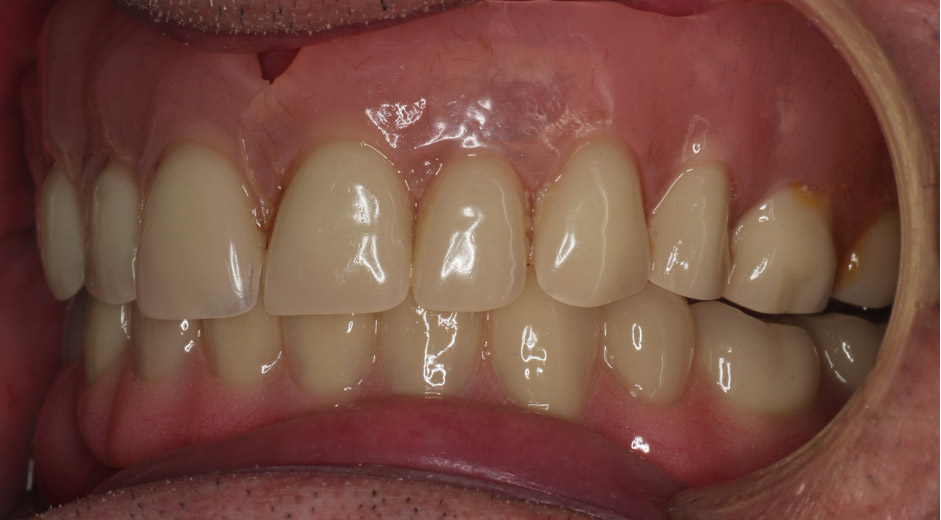
- Complete dentures
- Conventionally it is thought that bilateral balanced occlusion benefited complete dentures. However, this is not shown in the literature (Abduo, Tennant and McGeachie, 2013; Lemos et al, 2018; Zhao et al, 2013). Bilateral posterior balanced contacts in maximal contact position are far more important for denture occlusion (see Figure 4).
Designing occlusion with group function
Occlusal records required for accurately designing an occlusion with group function:
- Accurate impressions (digital or analogue)
- Accurate jaw relationship records
- Retruded (see Figure 5 and Figure 6)
- Protruded
- Intercuspal
- Facebow record.
The records of the teeth allow you to accurately assess and plan the anterior determinants of the occlusion. The jaw relationship records allow you to program the articulator to more accurately reflect the posterior determinant of the occlusion – the TMJ.
Prosthodontips question and answer section
This month we received the following questions.
When using the BEWE (basic erosive wear examination) is the score for each sextant due to erosion only, or all tooth wear?
This is a great question, and in this instance, the term ‘erosive tooth wear’ is confusing. Erosive tooth wear is another term for tooth surface loss and covers all forms of tooth wear. It is meant to cover the multifactorial nature of tooth wear, and also make note of the fact the tooth wear often has a component of erosion.
How do you know where to set OVD when reorganising a patient’s occlusion?
This is a very complex question, and could cover a whole series of columns. However, in very short terms there are a number of factors to take into account when deciding how much to increase OVD by:
- Amount of restorative space needed
- Planned position of incisal edges (guided by aesthetics)
- Incisal guidance angle
- Planned cuspal inclines.
Please keep the questions coming. You can contact us on Instagram (@sharplingdental and @prostho_zo) and also email (prosthodontips@googlemail.com).
If there are specific topics you would like us to cover in a column, please let us know.
Join us next month for the next instalment of Prosthodontips, where we will then discuss how to prescribe an aesthetic wax up.
Previous Prosthodontips:
Follow Dentistry.co.uk on Instagram to keep up with all the latest dental news and trends.
References
Abduo J, Tennant M and McGeachie J (2013) Lateral occlusion schemes in natural and minimally restored permanent dentition: a systematic review. Journal of Oral Rehabilitation 40(10): 788-802
Gross MD (2008) Occlusion in implant dentistry. A review of the literature of prosthetic determinants and current concepts. Australian Dental Journal 53(s1): S60-8
Kahn J, Tallents RH, Katzberg RW, Ross ME and Murphy WC (1999) Prevalence of dental occlusal variables and intraarticular temporomandibular disorders: Molar relationship, lateral guidance, and nonworking side contacts. The Journal of Prosthetic Dentistry 82(4): 410-5
Lemos CA, Verri FR, Gomes JML, Santiago Júnior JF, Moraes SLD and Pellizzer EP (2018) Bilateral balanced occlusion compared to other occlusal schemes in complete dentures: A systematic review. Journal of Oral Rehabilitation 45(4): 344-54
Manfredini D, Lombardo L and Siciliani G (2017) Temporomandibular disorders and dental occlusion. A systematic review of association studies: end of an era? Journal of Oral Rehabilitation 44 (11): 908-23
Zhao K, Mai Q, Wang X, Yang W and Zhao L (2013) Occlusal designs on masticatory ability and patient satisfaction with complete denture: a systematic review. Journal of Dentistry 41(11): 1036-42