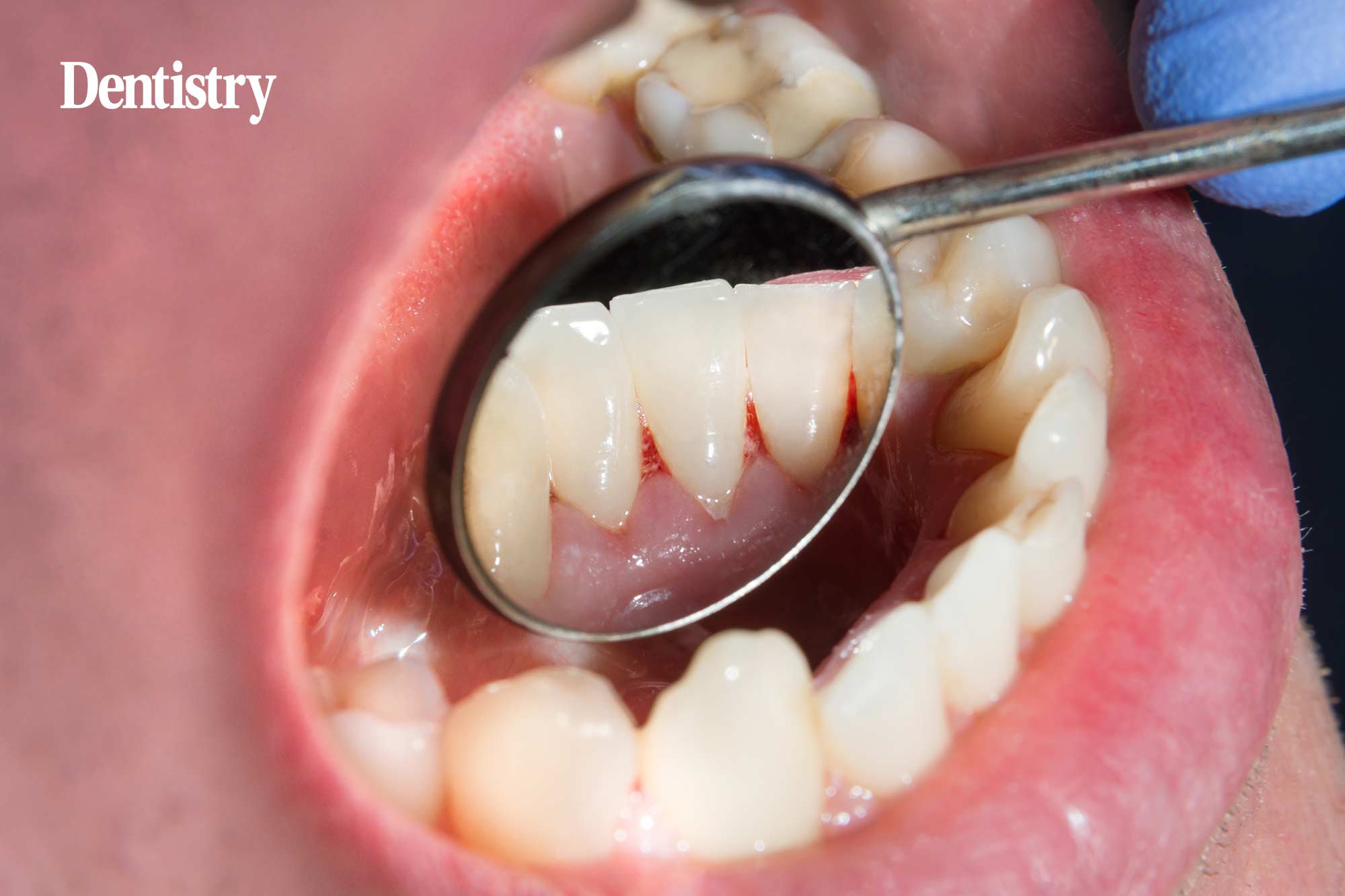
The second in a series of articles focusing on plaque biofilm, this instalment explores the issue of symbiosis and dysbiosis, as well as considering any association between oral and systemic health.
Brought to you by Johnson & Johnson Ltd, the makers of Listerine.
Plaque bacteria are considered a major cause of periodontal disease. It has been established that that good plaque control is an essential part of preventing gingivitis and periodontitis, which are a continuum of the same disease.
Tooth brushing and interdental cleaning are acknowledged as the mainstay of preventive oral care. But according to the Adult Dental Health Survey of 2009, 66% of dentate adults in England, Wales and Northern Ireland have visible plaque.
This is despite 75% of respondents claiming to brush their teeth twice a day. In addition, 25% report cleaning interdentally daily.
A multifactorial disease
Going straight to the heart of the matter, Chapple and colleagues (2017) wrote: ‘Periodontal diseases… are complex diseases with multiple and diverse exposures that impact upon risk of disease initiation (risk factors) or progression of existing disease (prognostic factors).
Exposures include those that are inherited (eg genetic variants), those that are acquired, such as social, educational and economic factors, and the local environment (eg biofilm load or composition), other diseases (eg sub-optimally controlled diabetes) and lifestyle (eg smoking, consumption of sugars, carbohydrate intake) factors.
These may arise in different combinations in different individuals, and at an individual patient level may also have differentially weighted effects.’
Chapple and colleagues (2017) continued: ‘… there is a symbiosis between a health-associated biofilm and a proportionate host immune inflammatory response. Periodontitis develops following the emergence of a dysbiosis in susceptible individuals which is associated with dysregulation of the immune-inflammatory response, and which leads to host mediated connective tissue damage and alveolar bone loss.’
The systemic link
At the 2017 World Workshop on the classification of periodontal and peri-implant diseases and conditions, it was stated that: ‘Periodontal diseases and certain systemic disorders share similar genetic and/or environmental etiological factors.
‘Therefore, affected individuals may show manifestations of both diseases. Hence, loss of periodontal tissue is a common manifestation of certain systemic disorders. [This] could have important diagnostic value and therapeutic implications.’
Offering further insight, Winning and Linden (2015) suggested: ‘Whilst there is now good evidence for periodontitis associating with various systemic diseases (particularly atherosclerotic cardiovascular disease and diabetes), evidence for a causative role is still lacking.
‘Many of the reviews in this area report that ‘further studies are needed’, but that should not prevent us taking a pragmatic approach in promoting a patient’s good oral health benefiting their general health.’
Taking early action
Tonetti and colleagues (2015) considered the importance of acting as soon as gingivitis has been diagnosed. They suggested: ‘Gingivitis and periodontitis are inflammatory conditions caused by the formation and persistence of microbial biofilms on the hard, non-shedding surfaces of teeth.
‘Gingivitis is the first manifestation of the inflammatory response to the biofilm. It is reversible (ie if the biofilm is disrupted gingivitis resolves), but if biofilms persist gingivitis becomes chronic. In some subjects, chronic gingivitis progresses to periodontitis.’
They further wrote: ‘Periodontitis is characterised by non-reversible tissue destruction. [This results] in progressive loss of attachment eventually leading to tooth loss.’
Therefore, if gingivitis is not resolved in a patient, it may develop into the irreversible, more destructive periodontitis, thus: ‘Primary prevention of gingivitis aims to avoid the development of more severe and widespread forms of gingivitis that may ultimately convert to periodontitis.’
In line with this need, the final instalment of this series of articles will investigate the latest evidence when it comes to disrupting biofilm, why it is so important, and how that might best be achieved by patients between dental hygiene appointments.
For further information, visit listerineprofessional.co.uk.
Read other articles in this series:
References
- Page RC, Kornman KS. The pathogenesis of human periodontitis: an introduction. Periodontology 2000 1997; 14: 9-11
- Kinane DF, Attström R. Advances in the pathogenesis of periodontitis. Group B consensus report of the fifth European Workshop in Periodontology. J Clin Periodontol 2005; 32(Suppl. 6): 130-1
- Chapple ILC et al. Primary prevention of periodontitis: managing gingivitis. J Clin Periodontol 2015; 42 (Suppl.16): S71-S76
- Barnett M L. The rationale for the daily use of an antimicrobial mouthrinse. JADA 2006; 137: 16S-21S
- Adult Dental Health Survey 2009. The Health and Social Care Information Centre 2011
- Chapple ILC et al. Interaction of lifestyle, behaviour or systemic diseases with dental caries and periodontal diseases: consensus report of group 2 of the joint EFP/ORCA workshop on the boundaries between caries and periodontal diseases. J Clin Periodontol 2017; 44 (Suppl. 18): S39-S51
- Albandar JM et al. Manifestations of systemic diseases and conditions that affect the periodontal attachment apparatus: Case definitions and diagnostic considerations. J Clin Periodontol. 2018; 45(Supp 20): S171-S189
- Winning L, Linden JG. Periodontitis and systemic disease. BDJ Team 2015; 2(15163)
- Tonetti et al. Principles in prevention of periodontal diseases Consensus report of group 1 of the 11th European Workshop on Periodontology on effective prevention of periodontal and peri-implant diseases. J Clin Periodontol 2015; 42 (Suppl. 16): S5-S11.

