In the first of the new column, Maria Lessani, president of the British Endodontic Society, discusses what you need to understand about the basics of endodontics to create a clear picture of the patient’s problem.
Endodontics 101 will cover the most basic endodontic knowledge that we, as dentists, are expected to know.
Most of this information was taught to us at undergraduate level. As newly qualified dentists we use these essential pieces of knowledge and try to get through each day.
This early period in our careers is a very challenging time, particularly around the discipline of endodontics. This was confirmed by many publications historically as well as by recent feedback received by the British Endodontic Society teacher’s group from foundation dentistry educators in Health Education England.
As experienced dentists, we often develop our skills by gaining further knowledge, eg from attending courses or our personal daily experiences (which includes making mistakes!)
Looking back at my early endodontic cases, I always learnt more from the cases where things went wrong, as opposed to those which went perfectly smoothy.
I soon learnt that things do not always go to plan. In my case, I realised it has something to do with a loss of focus, not drawing on knowledge of basic principles, not utilising my good habits into practice or being totally unprepared for a case that I probably should have not attempted in the first place!
First steps
The first step in improving the standard of endodontic care we provide is fully understanding the facts we learnt at dental school. Understanding why they were taught to us and why they matter.
A gentle reminder that understanding is a different principle to remembering facts and recalling them for exams!
Understanding allows us to show appreciation for the rationale behind each principle and apply it to the challenge at hand from basic principles. These principles can guide and improve us as clinicians.
In my experience the most common areas most dentists fall down on are;
- Misdiagnosis, mainly due to not listening to the patient’s symptoms or poor observation of clinical signs
- Not offering pulp therapy as the first option in suitable cases
- Not complying with aseptic techniques, including not using a rubber dam and contaminating the root canal system
- Poor length control because they did not take parallel radiographs using an aiming device (X-ray holder) or use an electronic apex locator. The role of both is essential for good length management
- Poor coronal seal, so the case is compromised
- Not following up cases to see the long-term outcome.
As an endodontic teacher for the past 20 years, I have realised there are certain areas that we need to know well, if we are to become comfortable with the disciple of endodontics. A few of the common difficulties we encounter as dentists are discussed below.
Diagnosis
When learning how to get a good pain history, some dentists are taught the commonly used pneumonic ‘Socrates’. This is very helpful as a prompt tool.
It stands for site, onset, character, radiation, associations, time course, exacerbating factors and severity.
We must gain information on the character of the pain – making sure we never say any words that describes the character ourselves. This is because the patient may be struggling to realise what the character of the pain is.
Often dentists are obsessed to see if a pain is sharp or dull, as textbooks have used these forever. As a result, these become the only words they use in their questioning.
Please stop doing this if you are getting in that habit. Remember, patients need time to think of the vocabulary that describes their pain. I often notice they need anything from five to 30 seconds to just think of the right words to describe the character.
I often ask: ‘What do you feel? How would you describe it?’ The word pain is not used either, as pain is perceptive. What is a niggle or tenderness to one person may be pain or sensitivity to someone else, so please be mindful of personal perceptions.
The word sensitivity can often be used by patients. For some it means sensitivity to certain agents, eg cold or hot, yet in others it means tenderness to palpation as they may be touching the tooth and it feels sensitive to them.
So please ask the patients what they mean by ‘sensitive’. Do not assume it always means the same thing to every single person. The basics of what brings on the pain and help it disappear, often referred to as aggravating and alleviating factors, is a great diagnostic tool.
Close inspection
During the pandemic, patients were often put on multiple courses of antibiotics. I found I met more people in this period that had taken antibiotics and not any analgesics.
In addition, some of them still had a lot of pain and no relief. This sadly made them ask for more antibiotics!
If a case has relief with antibiotics, we know we may be dealing with an infection. If it is relieved with anti-inflammatories and analgesics, we know we may have an inflamed pulp. And if none help, we may think of non-odontogenic causes.
Creating a picture of the problem
All this allows us to see a picture of the problem before we have even examined the patient.
Using special tests appropriately means always using the simple tools routinely and consistently. This includes using the periodontal probe to walk it around the teeth in the problem area to identify deep periodontal probing defect/pocket, wondering if there is a crack there.
Is there pus discharge from it?
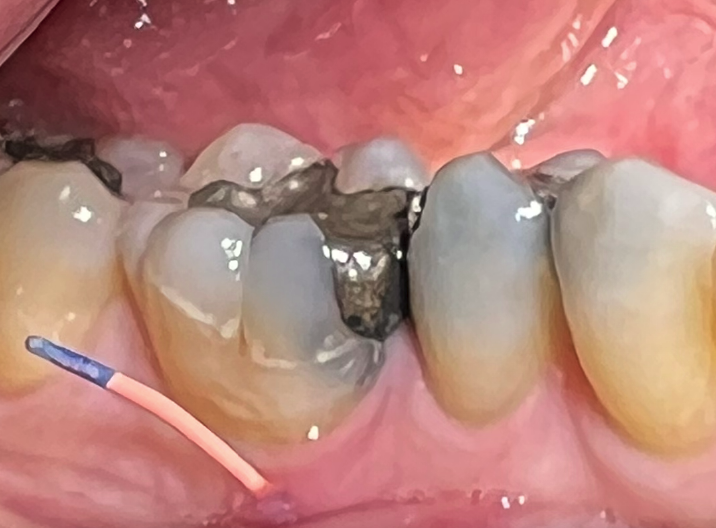
Not all sinus tracts are pedunculated through a patient reported ‘gum boil’. Remember if you see the latter, please trace it with a GP tracer. It may be sitting in front of one tooth and discharging from another! (Figures 1-2).
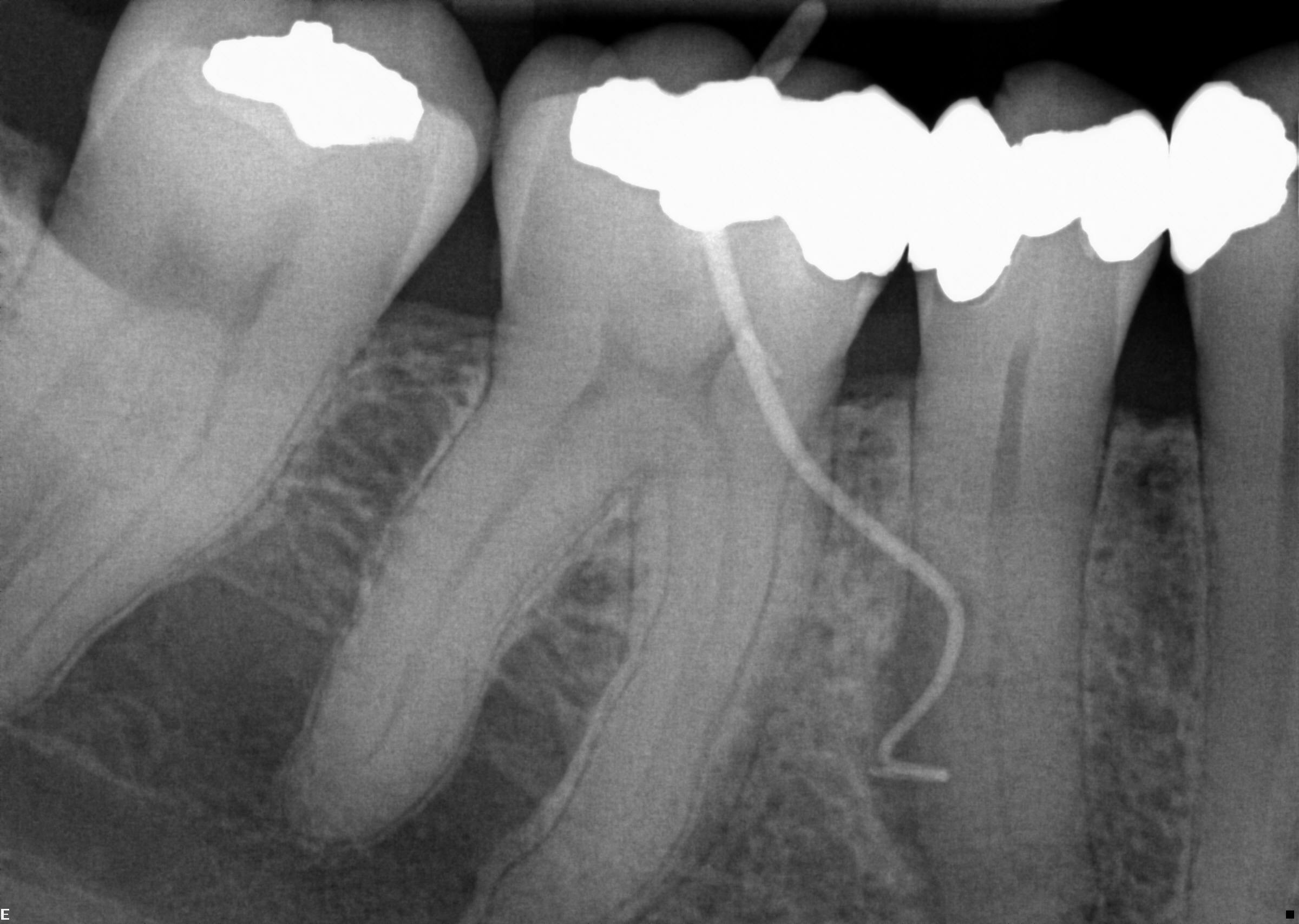
Take all bitewing and periapical radiographs with an aiming device, eg a Rinn system.
The bite test using tooth slooth is a helpful piece of plastic that could be on all examination trays (Figure 3).

This is another area where we are seeing more and more cases since the start of the pandemic. Is it related to more parafunction due to the wider world problem? Possibly!
Please use the tooth slooth to check each tooth and individual cusps in the area of the patient’s discomfort. Sometimes the culprit it is the cusp of a tooth you did not suspect.
Understanding the special test result
What is its relevance? The classic tenderness to percussion and palpation are often written down without us considering the pathophysiology of these.
It is important to think about what they mean. This can be caused due to different reasons. The dentist should be an investigator in trying to establish what these causes are.
Treatment is an area where we can improve in so many different ways.
In summary, this first column may highlight the areas where difficulties may be encountered and resources where further development can be sought.
The future columns will aim to address some of these in more detail.
What endodontic treatments can we provide for patients?
So often we forget about pulp therapy, eg partial pulpotomy.
Pulp therapy is aimed at saving the pulp in vital cases before we jump into root canal treatment! For example, management of deep caries and the exposed pulp.
Becoming aware of one’s own ability
It is important to know which cases are beyond one’s scope of practice.
There are tools that can be used to aid assessing the difficulty of cases to help identify if a case is beyond one’s management capability, eg the BES case assessment tool.
Understanding the crucial role of asepsis
So often we forget the cause of the disease is microbial and the aim is to remove it, eg using sodium hypochlorite as an irrigant.
It is sensible that we should pay more attention to disinfecting our gloves and rubber dam, placing our instruments on sterile trays during the appointment, correctly handling sterile paper points, disinfecting gutta percha points, and educating our nursing assistants on all of this.
Length control
This can be an area of stress for most dentists during endodontic treatment.
The aid of an electronic apex locator and radiographs taken using an aiming device eg Endo Ray (Figure 4), cannot be reinforced enough.
The various errors from blockage with debris through lack of adequate irrigation or forceful use of instruments are commonly the steps that need refining as they cause iatrogenic issues.
For example, ledging can cause length control problems.

Following up endodontic treatment
Following up endodontic treatment is imperative to this discipline.
After all the hard work, the success from resolution of a sinus tracts to radiographic healing should be important to follow ups. This is because we aim to understand our personal treatment outcomes.
This evidence can be utilised for better decision-making steps in planning for future cases. As an example, in some cases we appreciate our shortfalls and would consider referral or extraction more strongly, while in others we can value the simple steps to save pulps before offering RCT as an option.
How often and in what format following up is recommended is clearly reported in the European Society of Endodontology guidelines and referred to in the BES A Guide to Good Endodontic Practice.
Summary
In summary, these days there are so very many resources available to us to which we should refer to. We can often get overwhelmed!
The advice I give is to read and practice as much as you can, but please go to reputable sources for an evidence-based approach.
Follow Dentistry.co.uk on Instagram to keep up with all the latest dental news and trends.

