 Four months on from his open letter exposing the crisis in England’s NHS dental system, Tony Kilcoyne tells Sophie Bracken how bad the situation really is, and what should be done to turn it around.
Four months on from his open letter exposing the crisis in England’s NHS dental system, Tony Kilcoyne tells Sophie Bracken how bad the situation really is, and what should be done to turn it around.
On 4 January 2016 Tony Kilcoyne and over 400 colleagues from the dental profession published an open letter in The Telegraph newspaper, entitled ‘The NHS dental health system is unfit for purpose’. Calling for immediate government action to be taken, the letter said it is a ‘national disgrace that children aged under 10 in England are still more likely to be treated in hospital for rotten teeth than for any other medical reason’. This was the third such letter published by Tony and peers in The Telegraph in as many years.
The message from all three letters is clear: NHS dentistry in England is at crisis point, the result of dental system that is severely limited and incapable of providing the quality and quantity of care to patients that it claims to. Dentistry was keen to know what has made Tony and his colleagues whistle blow on their own profession for three consecutive years.
‘No one else is speaking out’, Tony told me. ‘People are afraid to rock the boat. They have contracts, targets to meet, their jobs depend on it – I get it, I understand. The NHS doesn’t like criticism, but we’re giving them solutions as well. If they took on board half of what we’ve said, it will improve things.
‘NHS dentistry in England is limited in resources, it’s limited in funding and it’s limited in what it can do for the population’, Tony said. ‘The problems all seem to stem from an extreme reluctance for the government to admit that.’
With three open letters to government in three years, chief dental officer for NHS England, Sara Hurley, has accused Tony and co’s actions as ‘unhelpful to the profession and patients’, and the assertions ‘difficult to substantiate’. Four months have now passed since the latest letter was published, and with the dust settling, Dentistry is eager to know what, if any, progress has been made.
‘Unfit for purpose’
Health & Social Care Information Centre statistics claim that in the two years to 30 June 2015, 30 million dental patients were since on the NHS in England, a 6.7% increase since 2006. As a percentage, however, this means that 55.7% of the population visited an NHS dentist in England between June 2013 and June 2015, a rise of just 0.1% since March 2006 (Health & Social Care Information Centre, 2015).
The report also states that in the two years to 30 June 2015, despite an actual rise in the number of children seen since March 2006 (up 2.5% to 8 million), as a percentage of the population, the number of children seen fell by 0.7% (Health & Social Care Information Centre, 2015).
‘What the figures really say’, says Tony, ‘is that slightly over half the population of England have had access to an NHS dentist. And by access they mean a single contact. Not necessarily a full course of treatment or getting them fully dentally fit and healthy, but at some point in the last two years they’ve had a tooth out in an emergency, or had one contact and were never seen again.
‘And that’s for two years. If you actually went to annual statistics, you might find that only a third of the population have seen an NHS dentist in one year. And then you have to ask, is that helping the health of the nation?’
Tony’s contention with these statistics doean’t only concern woolly access figures. The means of measuring ‘access’ is, in Tony’s words, ‘unfit for purpose’.
‘The government is perpetuating it’s own big lie to the public, that everything is available to everyone on the NHS, free regardless of income. Well it’s not available to everyone – we can hardly get half the population sorted. It’s not a service free for all, because the “tooth tax” as I call it, is now over £200 for the band three courses of treatment. On the NHS that is a phenomenal charge. I don’t know any other sector in the NHS that has charges that high.
‘So we have a situation where the government’s got addicted to collecting millions of pounds in tooth tax, and it needs a system that is related to collecting more money. And that’s the only thing that UDAs actually measure. The government loves UDAs, because it counts contact. The government can use statistics that don’t really reflect health, or quality of care or prevention, and the more UDAs that are done, the more tooth tax that’s collected. That’s the only direct correlation UDAs have with anything, how much tooth tax does it collect, and how many bodies have been rushed through NHS surgeries to collect that tooth tax.
‘They couldn’t tell you what treatment was needed, or how good that treatment is or how much prevention was done. They are nothing but a ranking system – small, medium, large – for the amount of tooth tax that is collected. Dentists recognise it, patients recognise it and the Health Select Committee recognised it. Yet here we are 10 years later with possibly the worst system in the world for dental health.’
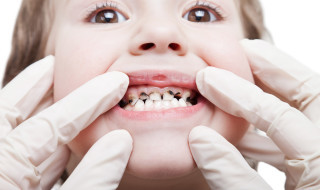
So what are the consequences of this system, 10 years down the road? ‘They’re all around us to see’, says Tony. ‘We have over the years seen rotten teeth going from the third most common reason for any child to be admitted to hospital in 2012/13, to now being the most common reason that any child is hospitalised under age 10. It is totally and utterly unacceptable.
‘Myself and 400 colleagues signed that letter in The Telegraph because we are appalled. There’s no good national strategy to stop what is in dentistry an almost totally preventable situation. It’s just disgraceful. I feel like I’m watching a slow motion car crash, and you’re thinking, someone needs to put the brakes on, someone needs to steer it away from the inevitable disaster.’
A proper national strategy
I asked Tony what his solution to this crisis would be. ‘We need a system that is prevention based, focused on the patient and most important of all, secures protected time for dental professionals to do their job well’, says Tony. ‘It’s as simple as that. Admit the system’s limited and reorganise it so it’s prevention- and patient-focused, not UDA targeted and collecting tooth tax-focused’.
This might sound simple, but this is only one part of Tony’s overall dental care strategy. Tony’s second target is to call on the food and drinks industry to take responsibility, and where appropriate, be held accountable, for the part it plays in damaging health – both dental and general.
‘We have to address the food industry – it is not doing enough self-control. Whether the government offers some kind of incentive to reduce sugar in foods, or also imposes some punishments, I don’t know. The end result we want is a lot less sugar being added to foods totally unnecessarily. A can of Coke does not need nine spoons of sugar to make it taste sweet.
‘What is surprising is – yes there are sweet foods and drinks, but it’s savoury foods that are having more and more sugar pumped into them. The food industry has found that if it adds sugar to things, it will sell more of them. Almost anything, whether it’s tomato ketchup, soup, bread or crisps’.
I ask Tony his opinion on the government’s plans to introduce a sugar tax in two years’ time. Does Tony believe the sugar tax would have a positive impact on reducing sugar consumption, as part of an overall healthcare strategy? Would taxation be an effective penalty for the food industry?
‘I don’t like calling it a sugar tax, because people are naturally going to think, “Oh no not another tax”, but if you have a can of Diet Coke next to a can of Coke the same size that’s got nine spoons of sugar in, the difference in price would let people know the health differences.
‘But I wouldn’t want to stop people’s choice to buy the can of Coke with nine sugars in. It’s about empowering the public to make the best choices. But we’ve got to hold [the food industry] responsible when things start getting so extreme.’
The third part of Tony’s strategy is to spread the oral health prevention message via the national media.
‘Because people cannot access dental care easily, and it’s more of a distress purchase and prevention isn’t as widespread as it should be, we need a national media campaign to inform the public on a few simple messages that they can do for themselves to prevent decay and gum disease’.
‘I feel like I’m watching a slow motion car crash, and you’re thinking, someone needs to put the breaks on, someone needs to steer it away from the inevitable disaster’
A media campaign, Tony says, would educate the general public on oral disease prevention. It’s an initiative that Tony believes would have widespread success: ‘The fire service did a media campaign to try and reduce the number of fires nationally. The government hailed it as one of the most successful public prevention campaigns that it has run. And it did it very cleverly with just a few million pounds, which in the scale of the whole budget to get everyone nationally preventing more problems, is good payback for the NHS.’
Tony suggests a national TV campaign backed up by radio and newspaper adverts and local area initiatives: ‘Three or four simple messages over the year about prevention, for children, teachers or doctors, social workers or everyday families. What if in two years’ time, only half the number of children were being admitted to hospital with rotten teeth? Wouldn’t that be a great thing?’
If a similar campaign worked for the fire brigade, there is no reason this initiative could not work for dental health. I expressed scepticism, however, on any governmental department agreeing to fund the project.
‘There could be an argument with NHS England, Public Health England, the Department of Health all saying they don’t want it to come from their budget’, concedes Tony. ‘But this is going to benefit all those departments to reduce the amount of disease, pain and burden on society. They need to get their heads together and say, “We’re going to throw a couple of million pounds at this”. What harm can it do? We’re only informing the public about self-help prevention messages. There’s no way people should be turning up at a dental practice and hearing prevention messages for the first time ever, like it’s a big surprise. We (dental teams) should be reinforcing existing messages and refining it for those patients.’
So that’s Tony’s three-point strategy to improve the nation’s dental health: a national media campaign backed up by local initiatives; address the food industry; and a dental system that’s fit for purpose that is centred on prevention and patients, not targets. ‘But all three have to come together’, says Tony. ‘At the moment everyone’s focusing on number three – minor changes to the contract. That just won’t do it. We need one, two and three working together – a proper national strategy.’
The ideal scenario
As Tony points out, the new prototype contracts include minor changes to the existing dental contract, not a significant system overhaul. If there is little change within the new system, what does Tony envisage for the future of NHS dentistry in another 10 years’ time, and what would his utopian scenario look like?
‘There’s a lot of short-termism in politics, and that’s a problem in itself’, he says. ‘But for health, I think 20- or 30-year plans should be made. And yes that includes dentistry. Dentistry needs to get the mouth back in the body so to speak, and needs to get back into the NHS.’
Tony believes that the government should admit that it is limited in its efforts to offer NHS dental care to every member of the population, and should instead focus on improving access and services where it can, whilst at the same time improving and promoting mixed and private dental services to bridge the gap.
‘Rather than be divisive – NHS versus private – it should be NHS and private, and give people more choices. Naturally some people will want totally private, and will pay privately or as part of a plan. Some will want to use mainly NHS, but might want some cosmetic work done, so might visit a mixed practice. Some people will use purely NHS services. Just give people the choice, but make all three services good – they all meet people’s needs in different ways’.
Action now
And so with the prototype contracts currently rolling out, it remains to be seen whether the blend A and blend B systems will offer more time for the dental team to promote the prevention message to patients, or if this new contract is just another ‘tooth tax’ collection in different clothing.
‘I just hope next year myself and hundreds of colleagues are not signing another letter at the beginning of January because nothing’s getting done’, says Tony.
Since the publication of the latest letter in The Telegraph on 4 January, over 8,000 children have been hospitalised for emergency tooth extractions, says Tony. ‘Every day we delay, more children are suffering, and it’s preventable. When are we going to do something?’
For references, contact [email protected].