In the Prosthodontips column this month, Josh Sharpling and Zohaib Ali discuss refurbishing an implant-retained bridge.
In the Prosthodontips column this month, Josh Sharpling and Zohaib Ali discuss refurbishing an implant-retained bridge.
As implant restorations become more and more common, the skill of refurbishing implant bridges (rather than replacing them) will become more and more valued by patients. I’ll discuss a case I completed recently and highlight my thought process.
Implant case presentation
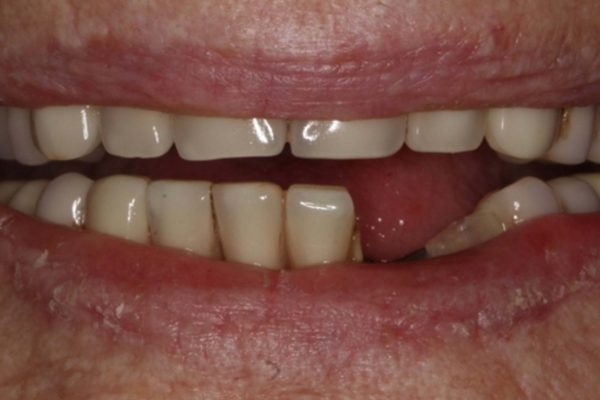
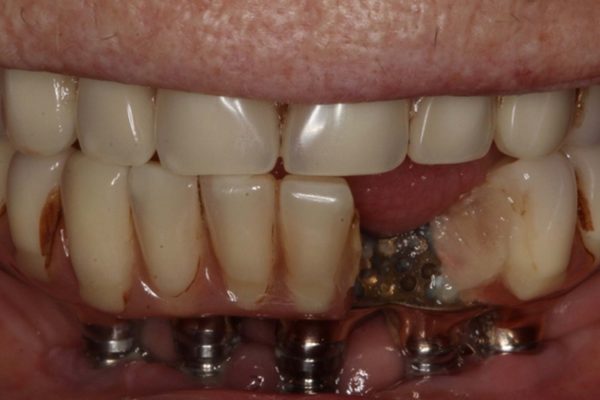
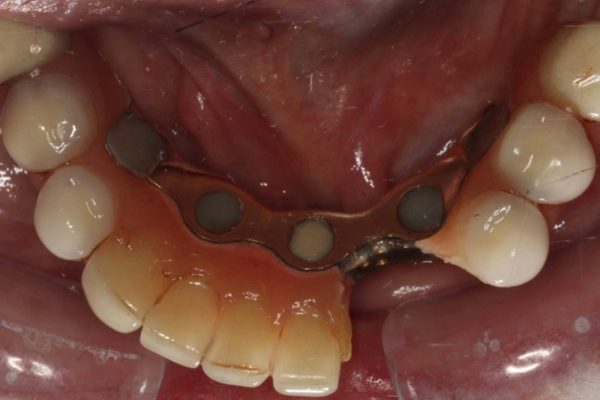
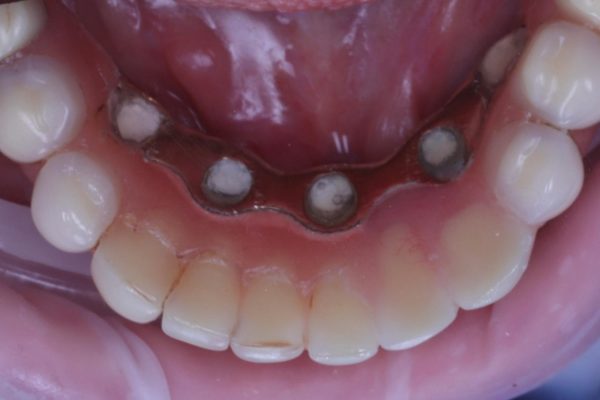
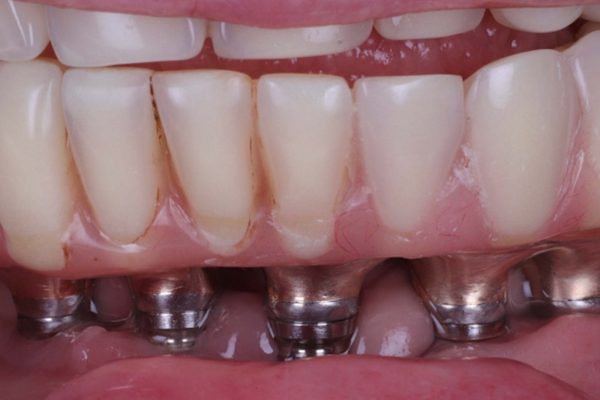
Figures 1-3 show a 90-year-old patient, who presented with a fractured 26-year-old implant bridge. This bridge has been in place for 24 years without incident. The patient was very happy with it.
Approximately two years ago some of the teeth fractured off. An intra-oral repair was carried out by the patient’s GDP. The patient was generally happy with this but always felt this area was a bit delicate.
When the area broke again, she came to see me for a more long-term solution. Her goals were: ‘I want my teeth back, and I want to be able to eat nuts without worrying about my teeth breaking’.
From my discussion with the patient, along with my assessment and radiograph (shown in Figure 4) I was able to find out this patient had been treated with Branemark implants, and the restoration was an acrylic bridge with a gold framework.
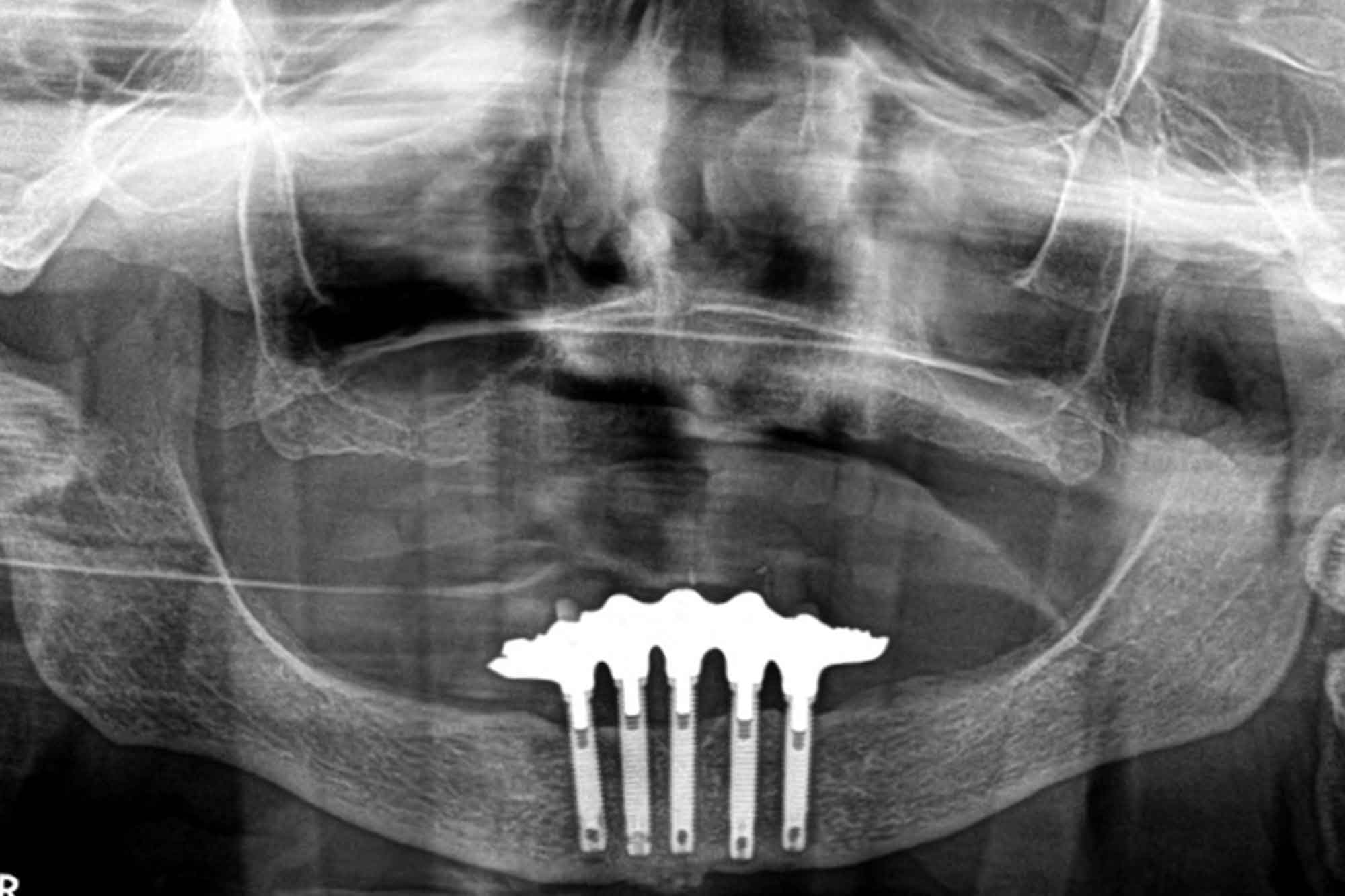
The bridge was occluding against a complete denture. This explains the minimal amount of wear present. This also makes me lean towards the idea that this bridge fractured due to fatigue of the acrylic, rather than the patient generating high occlusal forces (the amount of force able to be generated by a denture is far lower than with dentition, or fixed implants).
When I discussed the fracture with the patient, she advised me she always used this area to bite nuts.
Implant treatment options
Knowing the patient’s wishes there were three treatment options I recommended to the patient:
- A new implant-retained bridge
- Removing the acrylic from her current bridge, maintaining the gold framework, and fabricating a new acrylic teeth set-up
- Refurbishing just the fractured area of the implant bridge.
These are the other options I discussed with the patient but did not recommend:
- No treatment
- This does meet the patient’s wishes
- Explantation, and placement of new implants, and a new implant-retained bridge
- The bone loss and amount of thread show was coincident with the Branemark implants success criteria (bone loss to the first thread, and 1mm per five years after)
- An oral hygiene regime could be successful in maintaining these implants
- Removal of these long implants would be traumatic, and surgically complex, and this felt like an overly invasive plan in this case.
The patient did not want a new bridge and was worried about damage to the gold framework with extensive interventions. So she chose option three.
Difficulties
I anticipated the following potential difficulties with the treatment:
- Threaded screws, which would make screw removal much more difficult
- Screw fracture during removal
- Damage to the acrylic or the framework during removal and refurbishment
- Damage to one or more of the implants during bridge removal
- Finding that one or more of the implants was mobile once the splinting effect of the framework had been removed.
Therefore when discussing this option with the patient I advised them of the following risks:
- Damage to the implant bridge
- This may or may not be repairable
- Damage to the implant screws
- Spare screws would be ordered to replace any damaged screws as required
- Damage to the implants
- Mobile implants may necessitate their removal, and potentially require the placement of new implants and a new implant bridge.
Preparation
Before the appointment to remove the implant bridge, I accessed one of the implant screws – to confirm the screw head (and to ensure I had a driver which fitted this).
This also allowed me to identify the screws, and ensure I ordered the correct spare screws. As I was only accessing one screw; if the screw was fractured, or was damaged on removal, I felt confident the bridge could function with four screws in the short term.
On the day of refurbishment, I ensured that a local dental technician could repair the bridge on the same day. This meant the patient was without her bridge for only a few hours. This was vital for the patient and also eased a lot of her worries of being without teeth for a prolonged period.
Final result
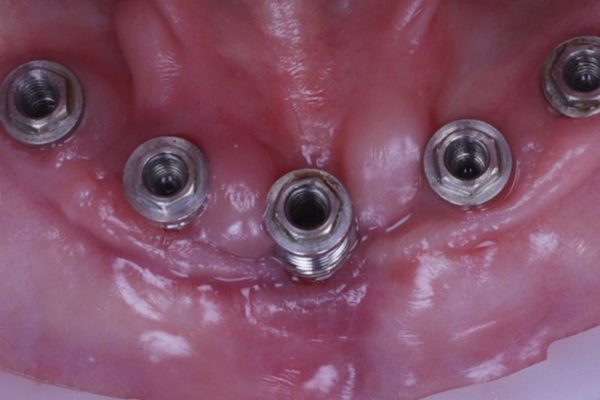
When the implant bridge was off, I was able to irrigate the area and remove the soft plaque deposits present (Figures 5 and 6).
The bridge was replaced, and then the screws torqued down to the manufacturer’s recommendations.
The occlusion and aesthetics were checked, and the patient was delighted that we’d managed to refurbish the bridge and achieved her goals. The final result is shown in Figures 7-11.
Please keep the questions coming for the Prosthodontips team. You can contact us on Instagram (@sharplingdental and @prostho_zo) and also email ([email protected]).
If there are specific topics you would like us to cover in a column, please let us know.
Previous Prosthodontips:
- Unstuck: composites
- Temporary crowns – not so temporary
- Canine guidance or group function
- Managing toothwear.
Follow Dentistry.co.uk on Instagram to keep up with all the latest dental news and trends.