 Lucy Nichols highlights some examples of best practise for cosmetic orthodontic patients
Lucy Nichols highlights some examples of best practise for cosmetic orthodontic patients
GDP orthodontics has revolutionised the way I work and I firmly believed it has enabled me to give patients superior treatment that is much more conservative than treatment I may have carried out in the past. However, there is much talk of the rise in litigation regarding GDP ortho. So in this article I am going to outline five key points which I consider are essential to carry out GDP ortho which is safe for both you and your patient.
1. Work within your competency
There are many one or two-day orthodontic courses out there aimed at GDPs. Don’t be fooled into thinking that in one or two days you can learn what orthodontic specialists take years to learn. After a short course you may be able to tackle some very simple cases. Over time and with continued attendance at courses your experience will grow and so will the number of cases you can take on. However, there will always be a good number of patients that you have to refer on.
2. Carry out a full orthodontic assessment
Many of the system-based short courses do not teach about orthodontic assessment. At the end of the day they want you to use their product and whether or not you experience litigation is not their concern. So if you haven’t been taught this on a course make sure you look it up and understand it. With a little practice it only takes a few minutes. You can have a printed template for your nurse to fill out, or you may be able to have a template on your computerised notes system that you can paste into the patient’s notes.
As a minimum you need to be recording the skeletal class, lower face height, FMPA (Frankfort-mandibular plane angle), lip competency and lip line, molar relationship, canine relationship, incisal relationship, overbite and overjet, degree and location of crowding or spacing, rotations or crossbites and habits such as tongue thrusting or thumb sucking.
A standard set of high-quality preoperative photos is of course essential. Remember to keep the study models for the required number of years.
However, other factors that are essential in orthodontic assessment, especially in adults, are recording their periodontal condition (BPE screen as a minimum), and a TMJ assessment. Obviously you are asking for trouble to start orthodontic treatment on a patient with deep perio pocketing. And a patient might only notice that asymptomatic TMJ click that they have always had, after their orthodontic treatment and attribute it to the treatment you provided. If you had failed to record this in your notes in your preoperative assessment if would be hard to prove that it wasn’t related to your treatment.
Pre-operative radiographs are important. However, it is also important to remember that every year there are a very small number of cancer deaths attributed to radiation from dental radiography. Therefore keep radiation doses as low as reasonably achievable (ALARA). If I have a patient with a sound or minimally restored dentition I will often wait until I have finished planning the movements to take radiographs. That way I can ensure I only take radiographs of the teeth that are to be moved. OPG radiographs give a useful overview but may provide insufficient detail to diagnose caries – additional bitewing radiographs may be needed as it would be unwise to commence orthodontic treatment on a patient with undiagnosed active caries. The radiation dose is likely to be lower with targeted periapical radiographs than an OPG and bitewings.
3. Individualised consent
I have worked with several orthodontic systems and they have all provided a standard consent form. I have never used these because they have lacked the space to write essential notes relevant to the patient’s specific case. I also feel they frequently contain dental terminology that is not understandable for patients and that this damages the legitimacy of the consent. So I transfer the information into my own Word document, change the language where necessary to make it a little more patient friendly and add several blank lines at the bottom just above where the patient will sign. Then in the surgery when we have discussed everything together, as they watch I write in any risks or compromises specific to their case. For example I may want to note that we are not intending to derotate a certain premolar, or we are not intending to correct a molar crossbite. Or I might write there is a small risk of the post crown with the short post debonding. I never use dental notation for the tooth. How does a patient know which tooth is LL3? So I would write this as ‘your lower left canine’. Then the patient will sign directly below this.
4. Record keeping
As the patient comes for their review appointment during their treatment it is essential to make the relevant notes. With removable appliances you will need to check compliance and with fixed appliances especially, to check their oral hygiene. Many cases will include interproximal reduction. I find this is most easily recorded on an IPR tracker which can be scanned into the patient’s notes at the end. It is also a good idea to take photos at review visits.
5. End of orthodontic treatment agreement
At the end of the orthodontic treatment it is a good idea to get patients to sign an end of orthodontic treatment agreement. This document is a statement that the patient is happy with the end result and accepts any compromises. Again there needs to be some blank lines to write in what these might be. You can use this space to again note the tooth in crossbite which has not been corrected. You may also note any black triangles that you have discussed and the patient is going to accept. You might also want to note compromises that were not planned at the outset.
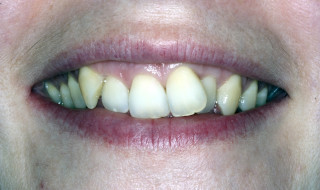
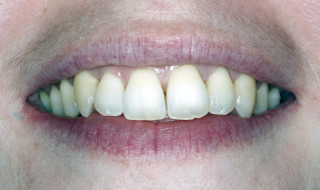
A patient who has had 12 months of Invisalign might not want a refinement even though you note that one tooth is a couple of degrees off the correct derotation. Such a case is shown in the photos (Figures 1 and 2). This patient was thrilled with the result at the end of her Invisalign aligners and declined a refinement because she was fed up with wearing aligners after one year of treatment, knowing she still had the retention phase to go. We discussed that a couple of her teeth weren’t in the perfect alignment but ultimately you can’t make a patient continue wearing aligners if they don’t want to. That is fine as long as you have discussed it with them and they choose to end treatment there.
The second part of this document contains instructions for the patient on wearing their retainer. They sign below to confirm that they understand what the requirements are for them regarding retainer wear and that they understand what the consequences may be if they do not follow the protocol you have advised.
Following these points should help aid communication with your patient in the first instance which is the most important factor in preventing litigation. If a case ever was pursued, with such water tight records you would certainly be in a much stronger position.
Lucy Nichols is a GDP in a private practice in Surrey with an MSc in resorative cosmetic dentistry and a keen interest in cosmetically focused orthodontics. She is also a committee member of the British Academy of Cosmetic Dentistry. She has worked with several orthodontic systems including the Inman Aligner, several clear aligners and fixed labial systems. She is currently undergoing further training in implant dentistry.
www.drlucynichols.com

