
The Aligner Dental Academy explains why periodontal health should not be overlooked when beginning orthodontic treatment.
The patient demand for straighter teeth continues to rise. However, as clinicians, we need to be mindful that orthodontic success is not defined solely by tooth alignment. True success lies in achieving results that are stable, biologically sound, and sustainable over time. When periodontal health is overlooked, aligner therapy can exacerbate underlying issues, leading to compromised outcomes.
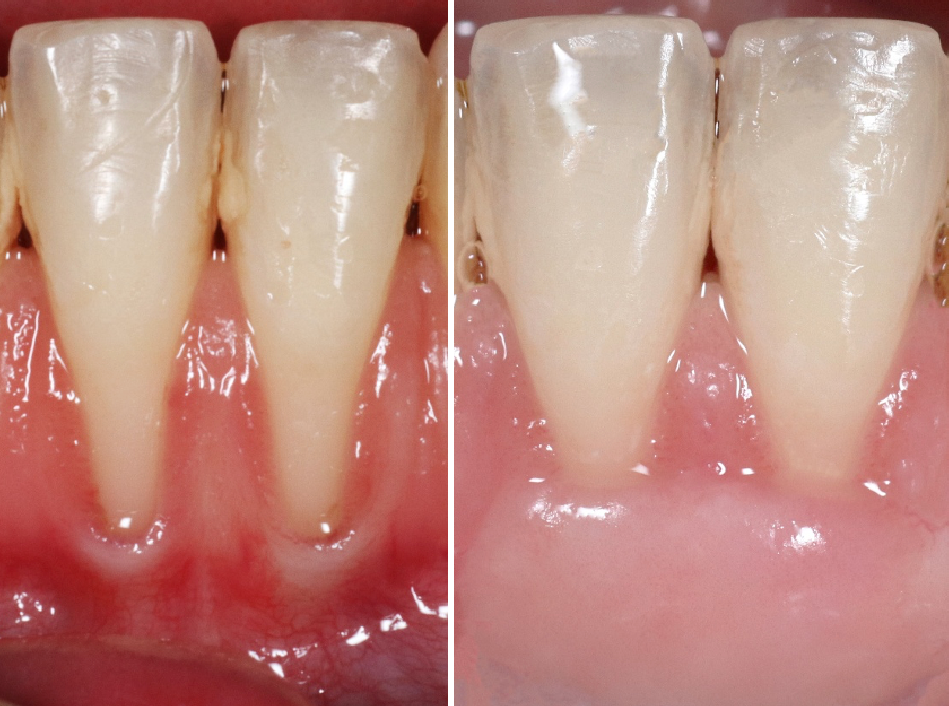
The starting point: periodontal stability first
One of the most common misconceptions in aligner therapy is that, because the forces are lighter and more controlled, treatment is inherently safer. While this may be partially true, it does not compensate for inadequate periodontal health at baseline.
Before initiating Invisalign treatment, clinicians must establish periodontal stability. This includes:
- Minimal bleeding on probing
- Controlled probing depths (ideally ≤4 mm)
- Good plaque control and patient compliance
- Stable radiographic bone levels.
Without these, even the most carefully planned aligner movements can lead to inflammation, attachment loss, and recession.
The key clinical shift is moving from ‘Can we align?’ to ‘Should we align, and is it safe to do so?’
Understanding the Biology
Clear aligners allow for precise digital planning, but biological reality still governs outcomes. Teeth do not move within software; they move within bone and soft tissue.
Patients with a thin gingival phenotype are particularly vulnerable during orthodontic movement. Even minor labial movements can result in recession or dehiscence. Aligner treatment does not eliminate this risk; in some cases, it may mask it due to its aesthetic nature.
Digital setups may suggest alignment, but the alveolar envelope must always be respected. Over-expansion or excessive protraction can push teeth beyond the bony housing, leading to long-term instability. These tooth movements require careful consideration in periodontally compromised patients. Even when delivered gently, these forces can accelerate breakdown if tissues are not healthy.
The role of pre-orthodontic periodontal intervention
In many cases, aligner therapy should not begin immediately. A structured preparatory phase may include:
- Scaling and root surface debridement
- Behavioural modification and oral hygiene optimisation
- Re-evaluation of tissue stability.
For high-risk patients, soft tissue grafting may be considered prior to orthodontic movement to enhance tissue thickness and resilience. Early referral to a periodontist can significantly improve both treatment planning and outcomes.
Aligners and oral hygiene: an advantage, if used correctly
One of the advantages of Invisalign is that aligners are removable, allowing patients to maintain better oral hygiene compared to fixed appliances. However, this benefit is entirely dependent on patient compliance.
Poor aligner hygiene or inconsistent wear can create a microenvironment conducive to plaque accumulation and gingival inflammation. Patients must be educated to:
- Remove aligners for eating and drinking (except water)
- Clean aligners regularly
- Maintain meticulous brushing and interdental cleaning.
In this sense, aligner therapy places greater responsibility on the patient, making case selection and motivation critical.
Long-term success over short-term aesthetics
Orthodontic treatment often concludes with visually pleasing results at debond. However, this is not the endpoint, it is merely a milestone. The true measure of success is stability years later.
Every course of orthodontic treatment introduces a degree of biological risk. Without ongoing supportive periodontal care, the likelihood of relapse, inflammation, and tissue breakdown increases. Regular maintenance, patient education, and long-term monitoring are therefore essential components of care.
Clinicians must shift their focus from short-term aesthetics to long-term health. This requires honest conversations with patients about risks, responsibilities, and the importance of maintenance.
Elevating outcomes through integration
When periodontology is integrated into orthodontic planning, the results extend beyond straight teeth. Function, aesthetics, and biology are all enhanced. The smile is not only aligned, but harmonised with healthy, stable tissues.
This interdisciplinary approach also reflects a broader trend in dentistry: increased accountability and collaboration. Digital planning tools have advanced significantly, but they cannot replace biological understanding. The principle that ‘digital planning does not equal biological planning’ serves as an important reminder that technology must always be guided by clinical judgement.
Screening tools, risk assessment protocols, and early specialist involvement should be a standard practice for delivering results that endure. iTero TimeLapse, part of the iTero intraoral scanner system, allows clinicians to compare sequential intraoral scans over time to visualise changes in tooth position and gingival levels.
For patients undergoing Invisalign treatment, it can be used before treatment to establish a periodontal baseline, during treatment to monitor for signs such as recession or inflammation, and after treatment to assess stability and outcomes. This is why using available digital tools like TimeLapse is highly beneficial, as it supports early detection, improves patient communication, and helps maintain periodontal health throughout treatment.
Ultimately, the integration of perio-ortho principles requires a shift in mindset. It is about recognising that the most critical factors in treatment success often lie beneath the surface. As clinicians, we must remain vigilant in assessing what cannot be seen at first glance.
This approach also reinforces the importance of patient selection and communication. Not every patient is an immediate candidate for orthodontics. Some require stabilisation, education, or adjunctive periodontal care before treatment can safely proceed.
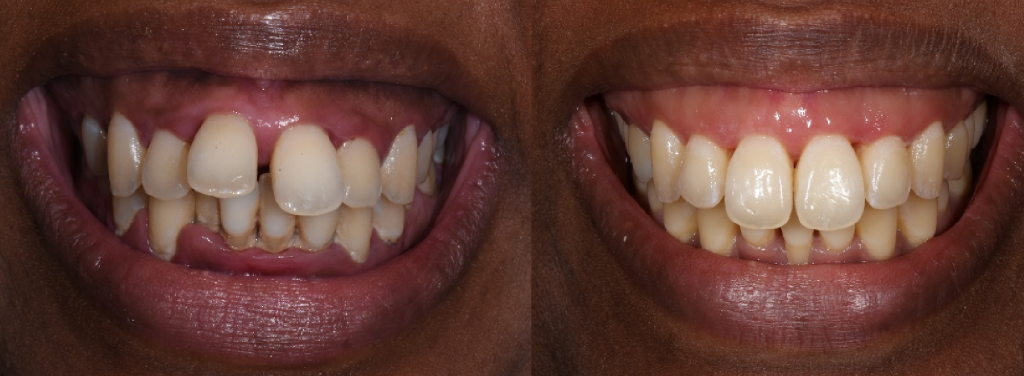
Conclusion
The relationship between periodontology and orthodontics is not optional; it is fundamental. By prioritising timing, respecting biology, focusing on long-term outcomes, and embracing interdisciplinary care, clinicians can significantly improve treatment predictability and patient satisfaction.
As the profession evolves, the emphasis must remain on delivering care that is not only effective, but responsible. Straight teeth are important, but healthy foundations are indispensable.
The future of orthodontics lies not in moving teeth faster, but in treating patients more safely, and that begins with ensuring long-term periodontal stability.
This article is sponsored by Aligner Dental Academy.

