
Over the past couple of years you will no doubt have read numerous articles outlining some of the day-to-day failures seen within the NHS (some even by myself, perhaps). Whilst the difficulties have been much publicised, many of the things we get right are often forgotten and, dare I say it, taken for granted.
The advantages of the NHS are even more noticeable when looking at third world countries, where a lack of basic provisions often results in the spread of disease considered eradicated in the west.
Let me turn your attention to the work of the charity Mercy Ships, which provides free medical and dental care to areas of the world not fortunate enough to have a system like the NHS.
Mercy Ships comprises a fleet of hospital ships that have been visiting developing nations since 1978 and are crewed by volunteers offering healthcare and other professional services free-of-charge.
Many people in developing countries have never had the opportunity to see a dentist. Dental care is almost non-existent in much of west Africa, as well as many of the other areas the ships visit. In common with many industrialised countries worldwide, the most frequently seen oral diseases are dental caries and periodontal disease. However, unlike many countries, thousands of people suffer from dental pain for weeks, months, sometimes even years, because of the lack of available dental care. Whilst accessing NHS services can lead to difficulties for some patients in some areas, in the UK we rarely hear of death as a result of untreated dental infections. Consultant oral and maxillofacial surgeon, Mr Leo Cheng, who regularly volunteers at Mercy Ships, informs us that in the third world, dental infection can, and does, kill.
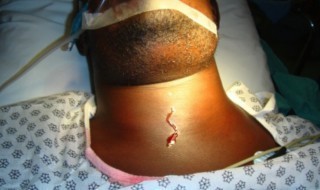
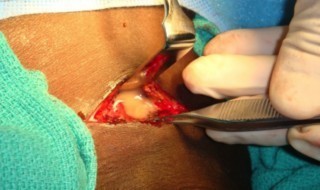
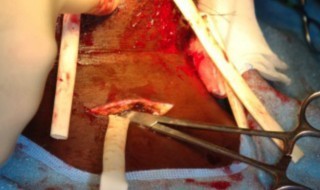
Through the direct lack of healthcare at an early phase the patient in first images required life-saving emergency treatment as a result of a spreading dental infection. Drains were inserted in all facial spaces in his neck and the floor of the mouth, and regular irrigation through the drains with antiseptics (ie, betadine, hydrogen peroxide, etc) was necessary to wash out abscess cavities within his chest. Thereafter, this patient was intubated in ITU (intensive therapy unit) and was kept in ITU for three days before extubation. He continued to receive irrigation of his mediastinal abscesses for another two weeks before his infection was under control.
Providing first class dentistry in the third world
Onboard, the volunteer dentists, nurses and hygienists play an important role in the prevention of dental diseases and help educate patients by showing simple oral hygiene tips, as well as by introducing fluoride to the oral cavity. Whilst many patients have to undergo procedures, such as the extraction of teeth and roots, dentists are also able to restore teeth with composite fillings. Mr Cheng also informs us that at one point dental students had come on board to observe Mercy Ships in action, in the short time they were there volunteers ended up extracting more than 90 roots and teeth, more than required for their entire dental training.
Deformities in developing nations

For the poor in developing nations, accessing necessary medical and surgical care is extremely difficult due to their remote location, lack of medical facilities and financial constraints. Conditions that would be treated in the early stages in developed nations grow to the point of being life-threatening. The consequence for many is a lifetime of disability and rejection.
Cleft lip and/or palate is a condition easily repaired in the developed world, but cleft lip babies born in developing countries are often malnourished because they cannot feed properly. Children who do survive are often rejected because of their deformity. The statistics tell us that cleft lip and palate is the number one facial birth defect and the fourth most common birth defect overall, affecting one in 700-1,000 live births.
In the UK, cleft lip and/or palate is routinely treated at a young age, but in west Africa this can be seen into adulthood. In west Africa superstition also plays an important role in how children with facial deformities are treated. I am informed that many children with this condition are kept hidden from view, rejected by friends and family, stoned if they appear in public and in some cases have been buried alive.
The lack of healthcare provision and education has meant that in many cases witch doctors or village chiefs are often the first port of call for many local villagers. Unfortunately the advice given can have disastrous consequences for those affected. Rather than recognising these conditions as defects that may be corrected through surgery, often the cause is put down to the devil or to evil spirits. Much of the advice given is based on local superstition and a real lack of healthcare access means that, for many, there is no option other than to take this advice.
Humphrey Hawksley reported for the BBC that, whilst billions of dollars of aid have been invested in schemes to modernise Africa and end poverty, traditions such as secret societies and witchcraft are still deeply entrenched and often pitted against what the west is trying to achieve there.
If you are interested in learning more about the work provided by Mercy Ships please visit www.mercyships.org.uk, where you will be able to find more information and some truly heartwarming stories about some third world citizens not lucky enough to have access to proper healthcare, let alone a national health service. Photos courtesy of Mercy Ships UK.

