Follow Dentistry.co.uk on Instagram to keep up with all the latest dental news and trends.
 In this month’s Prosthodontips, Josh Sharpling and Zo Ali discuss toothwear, how to diagnose it and how to treat it.
In this month’s Prosthodontips, Josh Sharpling and Zo Ali discuss toothwear, how to diagnose it and how to treat it.
Toothwear, tooth surface loss, erosion, attrition, abrasion, abfraction. There are many ways to describe the non-carious loss of enamel and dentine (Figure 1).
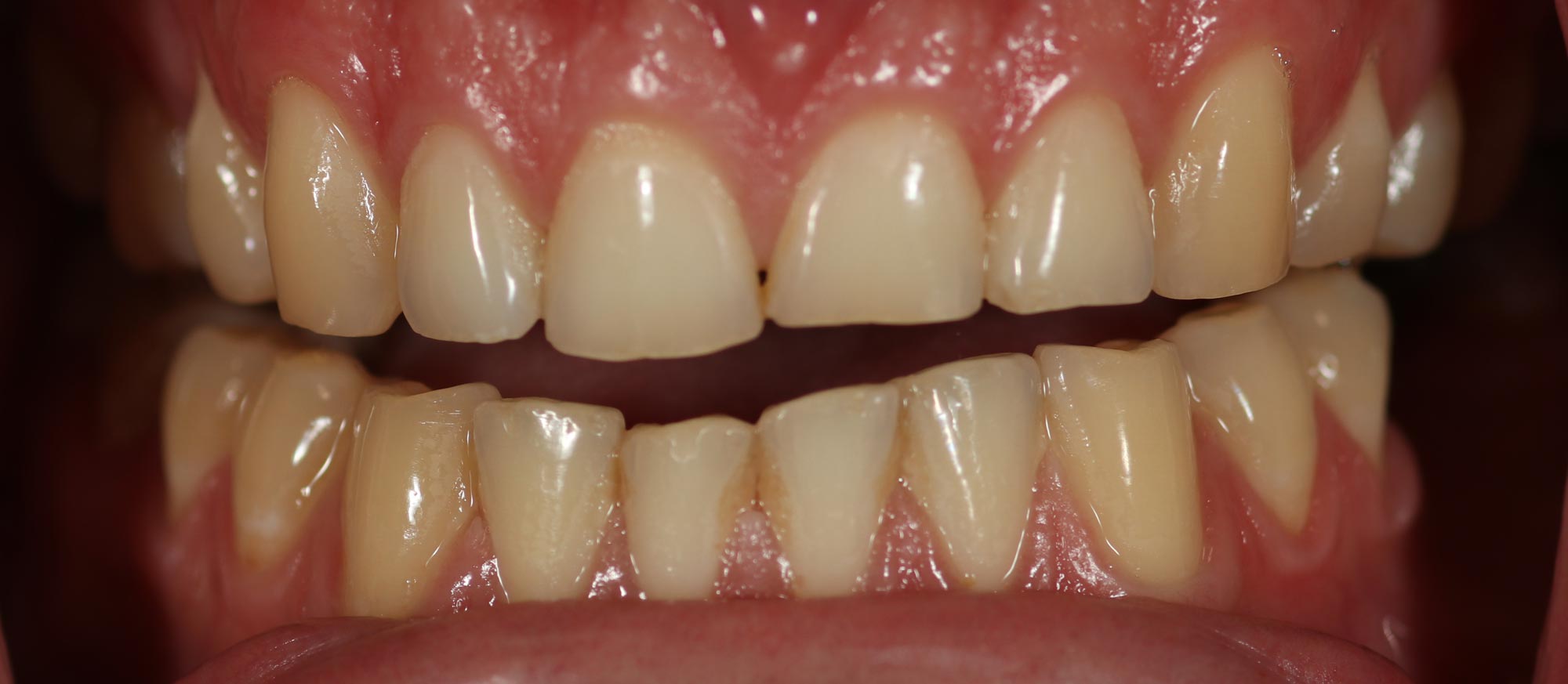
The terminology has evolved as our understanding of the microprocesses involved has improved. One thing, however, is for certain: toothwear is on the rise.
Over three-quarters (77%) of dentate adults displayed toothwear in their anterior teeth according to the 2009 Oral Health Survey. And the overall prevalence of moderate wear increased by more than one third in the previous 11 years.
What does this mean for our daily practice?
Patients with toothwear can present with a wide range of complaints. Especially those who are new to your practice or have not been for a dental visit in some time.
The specific clinical presentation may relate to the severity of the toothwear (eg fractured incisal edges or dentine hypersensitivity). But sometimes the patient may complain of more vague symptoms, which eventually lead to diagnosis of toothwear (eg cracked tooth).
Commonly the first complaint is aesthetic in nature – the patient will complain of short teeth, or thin teeth.
In our experience, many patients have remained undiagnosed or unaware of their condition. This presents an invaluable opportunity to build rapport with the patient and gain their confidence, through an accurate diagnosis, along with an explanation of their symptoms.
In this month’s column, we are going to explore the causes and essential management of toothwear. Before diving deeper into interceptive care later on.
Once you understand and can differentiate between the various aetiologies, the treatment options become apparent. And the decision-making process is simplified.
Aetiology
One of the most important factors, if not the most important, in successful management of toothwear is figuring out the cause.
It’s also important to remember that toothwear is a normal physiological process that occurs over time. Therefore we must make an assessment to differentiate between physiological and pathological loss of tooth substance.
To define it as pathological, we must observe a negative effect on function or aesthetics; or we predict the tooth will not survive the current (accelerated) rate of wear.
There are three general causes of toothwear: erosion, attrition and abrasion. Abfraction is as yet not fully proven and its role is contentious.
Most patients will present with a multifactorial condition, commonly a mix of erosion and attrition.
It is our role to try to identify the causative factors which led to this and which aetiology (if any) has primarily contributed to the toothwear.
Dental erosion
Dental erosion is essentially dissolution of the enamel and dentine due to a chemical process.
Acid from intrinsic (the stomach) or extrinsic (dietary or environmental) sources cause initial softening. After which another acidic exposure results in total loss of the superficial layer of enamel.
Erosion is also responsible for the hypersensitivity that some patients present with.
The source of the acid is very important. Erosion on palatal surfaces of maxillary teeth is likely to be due to intrinsic acid. It is therefore suggestive of gastro-oesophageal reflux disease, rumination or other eating disorders such as anorexia nervosa and bulimia nervosa (Figure 2).
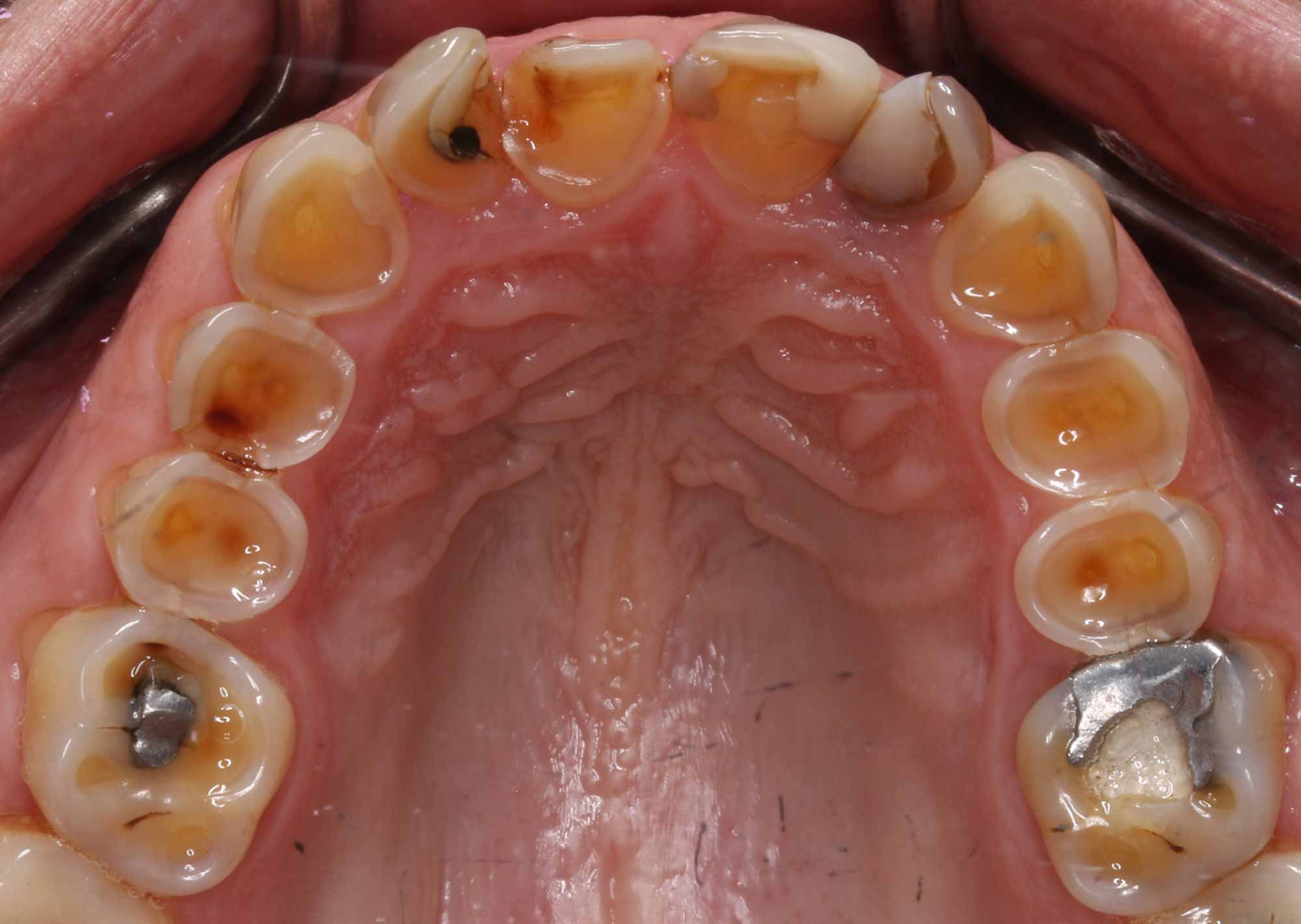
Labial and buccal lesions are generally more likely to relate to dietary components (Figure 3). Foods with the highest erosive potential include citrus fruits, apples and grapes. These are followed by soft drinks, alcohol and carbonated water.
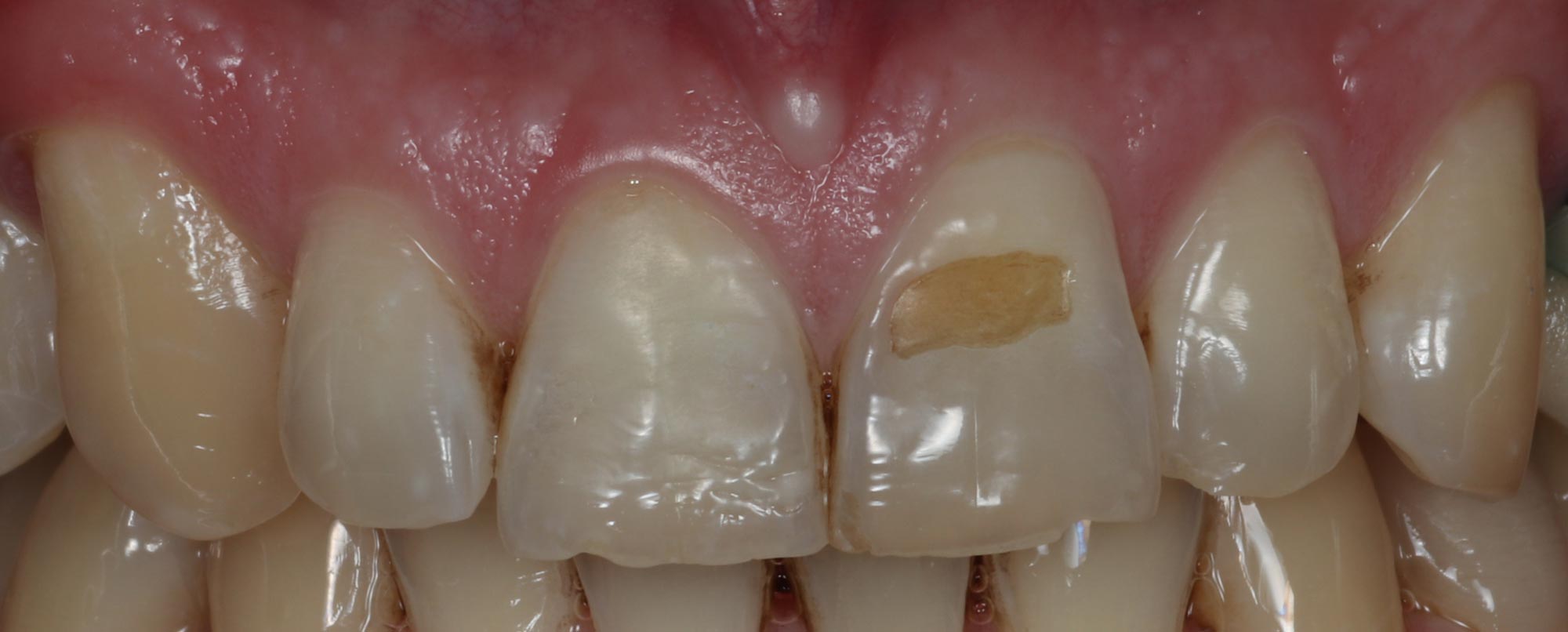
Recent research shows that increased frequency of these foods and consumption between meals greatly increases the damage they can cause.
Dental attrition
Dental attrition is the loss of tooth structure due to friction between opposing teeth (Figure 4).
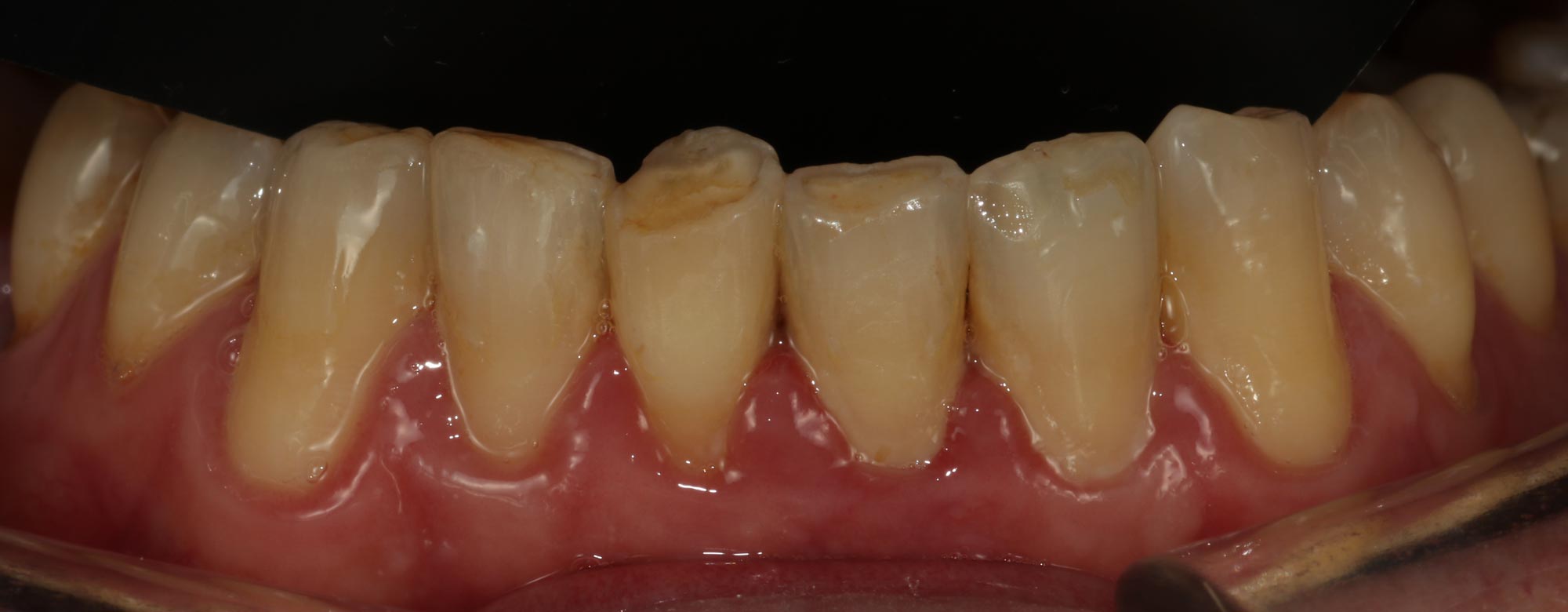
In normal function our teeth are thought to contact for only 17.5 minutes daily. However, increased contact, as occurs during parafunction, can cause attrition.
Parafunction can include any habit not related to normal oral function. This includes nail biting, pen or pencil chewing, using our teeth to cut or tear packaging and bruxism.
Bruxism is obviously the most commonly noted factor with relation to attrition. But the others are certainly worth bearing in mind (as causes of abrasion), especially for localised defects.
It is important to note that bruxism can occur both at night or during the day. This has an impact on treatment decisions further down the line.
Dental abrasion
Dental abrasion is the wearing away of a substance through some unusual or abnormal mechanical process. Generally we see this as toothbrush abrasion causing cervical lesions of teeth.
As mentioned above, most patients display multiple aetiologies and so the clinical picture is often somewhat muddled.
Tooth wear of multiple aetiology will often occur at a much increased rate (especially a combination of attrition and erosion). A new terminology has emerged and Lussi and Carvalho (2014) conclude that: ‘The terms “dental erosion” and “erosive toothwear” should be used to refer to the chemical and chemical-mechanical processes, respectively.’
What to look out for
It is easier to break up clinical features into anterior and posterior teeth. Then further break it up into early signs and later signs of erosive toothwear. On anterior teeth, look out for:
- Initially enamel with glassy appearance
- Visible colour differences (indicative of enamel thinning or frank dentine exposure)
- Progressively, there may be loss of palatal enamel from maxillary anterior teeth (intrinsic acid)
- Thinning or fractured incisal edges (Figure 5).
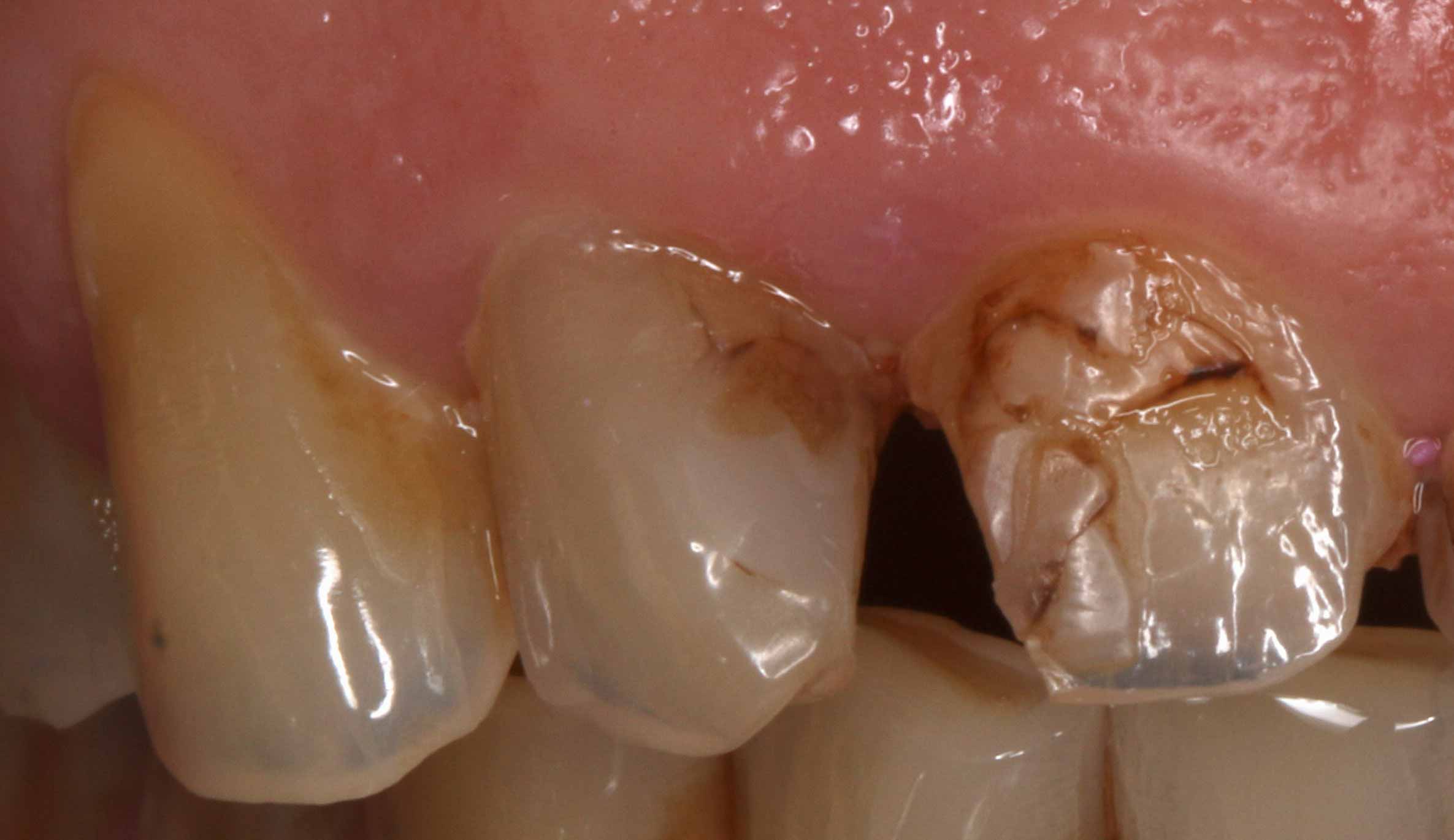
Posterior teeth also display some specific features which are helpful in diagnosing the condition:
- In the first instance, a few small round lesions which appear unthreatening
- Progression of these lesions leads to characteristic ‘cupping out’ lesions
- These lesions may then combine to cover most and eventually all of the occlusal surface (Figure 6)
- Restorations may stand proud of the adjacent enamel and dentine as they are not prone to the same degradation.
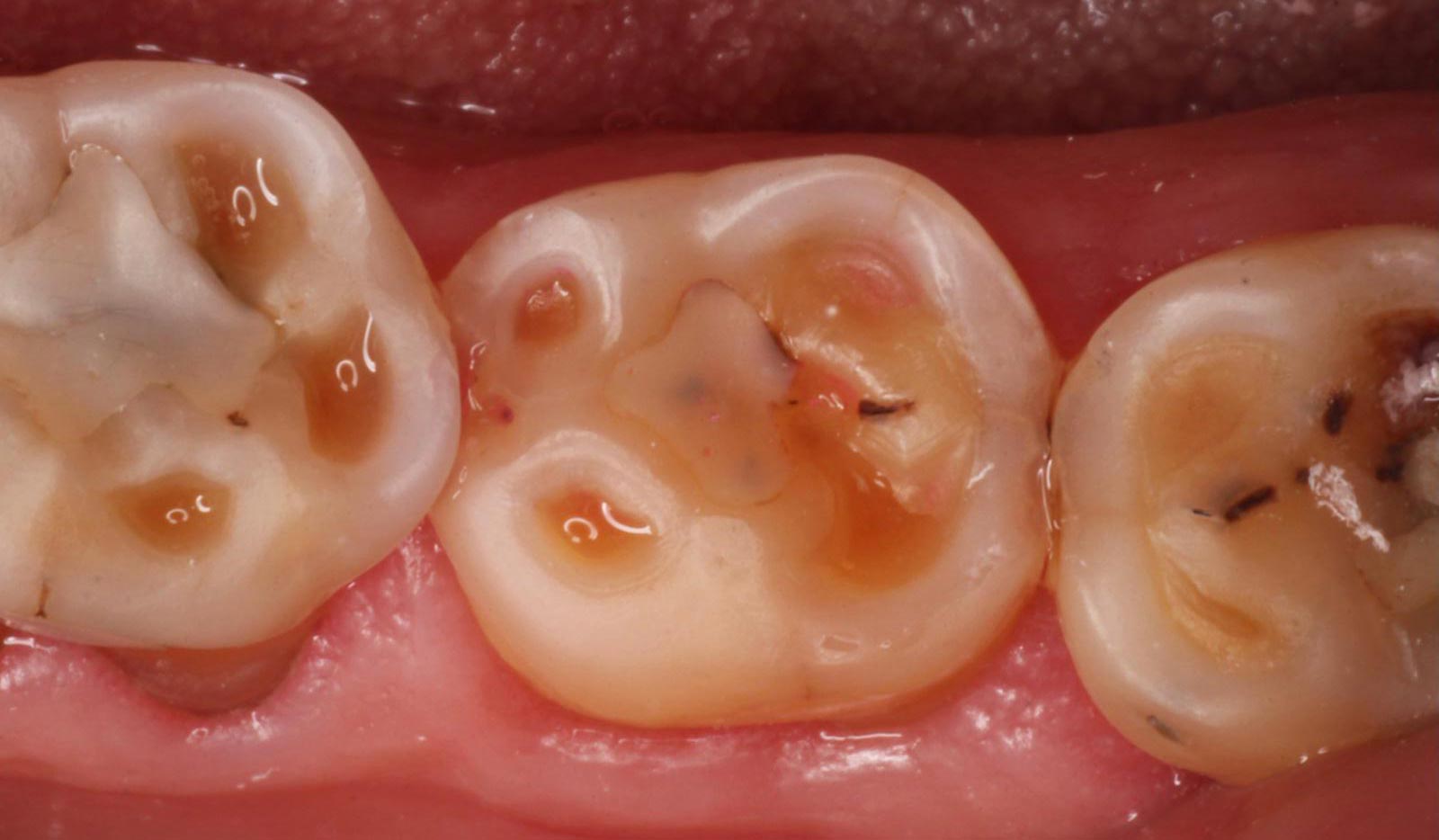
If there are matching wear facets on teeth, then clearly attrition is playing a significant role. If however the worn surfaces do not touch in maximum intercuspation, we would be almost certain that there is a predominantly erosive component to the aetiology.
As mentioned, most cases have a combined aetiology (Figure 7).
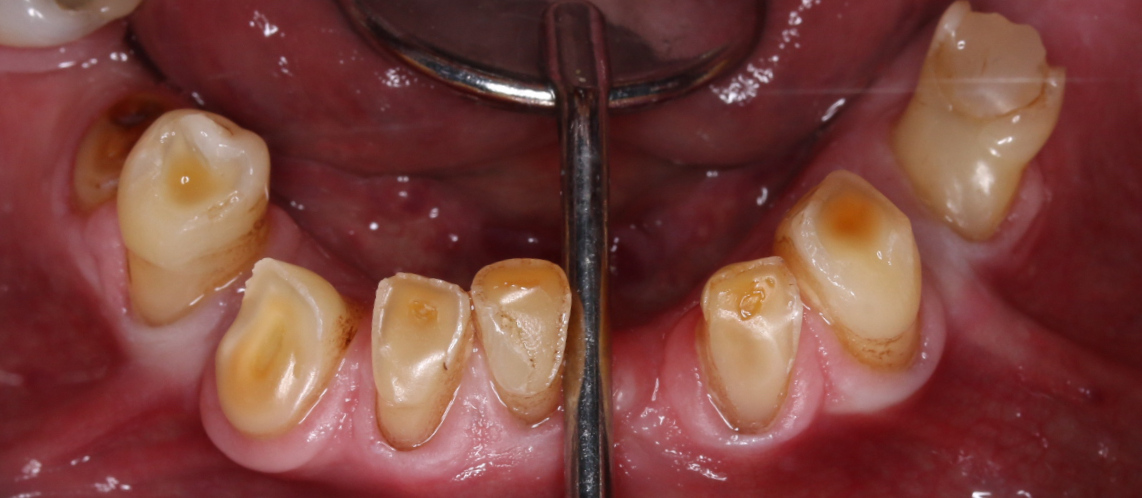
How do we manage our patient?
Thankfully there is a systematic way to manage almost any patient who presents with erosive toothwear. It is not that different to any other condition.
As with diagnosis and aetiology above, it is good to have a system to ensure nothing is missed. But also to allow the patient to take ownership of the problem.
- Address the initial complaint
- Make an accurate diagnosis
- Analyse all factors leading to diagnosis
- Implement a stabilisation regime
- Restore aesthetics and function as appropriate.
Initial complaint
Generally, this is either aesthetic (eg short or broken front teeth) or functional (eg sensitivity or cracked teeth).
Aesthetic concerns are usually difficult to address immediately because of the effects of toothwear on occlusion.
Sensitivity is best managed through the appropriate use of fluoride and dietary modification. Dentine bonding agents or covering dentine where occlusion allows is also reasonable at this stage.
Making an accurate diagnosis
Use the descriptions of the aetiologies above to arrive at a diagnosis.
Look closely at the patterns and location of wear defects to determine if acid is likely to be intrinsic or extrinsic. Watch out for matching wear facets to determine whether attrition is a factor.
If your patient is currently experiencing sensitivity, it is an indicator that erosion is active. Conversely, if you note stains on worn surfaces, it may indicate the tooth wear process is currently less active.
Your diagnostic statement should include aetiology, severity and extent of tooth wear (generalised versus localised).
Severity is difficult to gauge but there are a number of indices out there such as the Basic Erosive Wear Examination (BEWE) and the Anterior Clinical Erosive classification (ACE) to help guide you.
Your diagnosis should look something like: ‘Moderate generalised erosive toothwear with localised severe lesion affecting the anterior teeth.’ This level of clarity also helps with the treatment planning process.
Analyse all toothwear factors
Essentially, we must ensure we have turned over every stone to determine which factors are contributing to the patient’s condition.
It is worth asking the patient to complete a seven-day diet diary and we would routinely use this in our daily practice. This also helps to get the patient to emotionally buy into their own care and take ownership of their erosive tooth wear.
Stabilise your patient
This means removing causative factors or at the very least mitigating against them.
Use of fluoride, dietary modifications, behavioural and lifestyle changes and use of an occlusal splint (this may be contraindicated in a patient with uncontrolled gastro-oesophageal reflux) are all very reasonable approaches.
Manage each contributory factor and thus the patient will begin to understand what has happened over time. This will also produce results such as reduced sensitivity which patients will eventually pick up on.
Restore the dentition
This is case specific and requires extensive consultation and diagnostic work.
Virtually every case will require mounted study models with wax ups and/or denture set up to aid planning and communicate the treatment plan to the patient.
We will discuss restoration in subsequent articles as it is a lengthy subject.
Prosthodontips
Please do get in touch with us at prosthodontips@googlemail.com if you have any questions about erosive tooth wear, or prosthodontics in general.
We are also happy to answer case-related questions. Below is a question we received after the last Prosthodontips article.
Is there any toothpaste which is better for patients with erosive tooth wear?
The answer is yes; lots of different toothpastes are beneficial. Sensitive toothpastes are useful in managing patients with sensitivity in the first instance. We can also prescribe high fluoride toothpaste to promote remineralisation of the erosive lesion.
There is some evidence that the type of fluoride in the toothpaste can also make a difference; toothpastes containing stannous fluoride are shown to give more protection from an acid attack, in comparison to those containing sodium fluoride.
References
Bartlett DW (2005) The role of erosion in tooth wear: aetiology, prevention and management. Int Dent J 55(4 Suppl 1): 277-84
Jordão HWT, Coleman HG, Kunzmann AT and McKenna G (2020) The association between erosive toothwear and gastro-oesophageal reflux-related symptoms and disease: A systematic review and meta-analysis. J Dent 95: 103284
Walton TR (2013) The up to 25-year survival and clinical performance of 2,340 high gold-based metal-ceramic single crowns. Int J Prosthodont 26(2): 151-60

