NSK explains how minimally invasive dentistry is transforming prophylaxis and periodontal care through technologies like air polishing, powder therapy and piezo systems.
Minimally invasive dentistry in focus
Minimally invasive treatment has received increased attention, especially in periodontitis treatment and prophylaxis. The goal of minimally invasive treatment is to preserve healthy tissue and reduce pain and recovery time. Ideally, patients will experience the benefits of this approach, making it easier for them to engage in the preventive care we offer in dentistry.
Modern technology: airpolishing, powder therapy and piezo
Prophylaxis is gaining increased attention, and the demand for modern, minimally invasive equipment has increased.
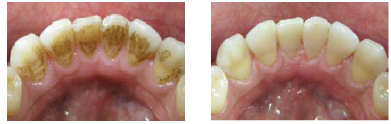
Airpolishing
Air polishing technology was first developed in 1945 by Dr Robert Black, originally using aluminium oxide for tooth preparation. In the 1970s, it became popular to remove discolouration using a gentler powder, mainly for use supragingivally. Air polishing was previously seen as a cosmetic treatment, but today it has an important role in pathological treatments, in the form of powder therapy and biofilm removal.
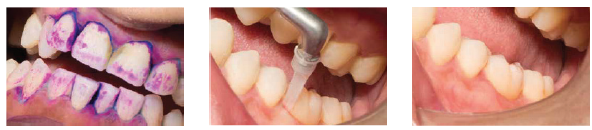
Powder therapy: a breakthrough in biofilm removal
In the 1990s, the development of biocompatible powders began, and research looked at the potential of air polishing technology to remove biofilm. The development of new powder types and lower-pressure technology enabled both sub and supragingival treatment, throughout the mouth, making treatment more preventive and pathologically directed.
In the late 2000s, subgingival air polishing was introduced as a new treatment modality. The method was initially a revolution in implant maintenance and peri-implantitis prevention but has since proven to be highly effective for full mouth debridement – including biofilm removal on gingiva, tongue, mucous membranes, furcations, crowns, bridges and root surfaces.
The powder, which consists of amino acids, the body’s own protein, is biocompatible and gentle while effectively removing biofilm and light discolouration. The fact that the powder does not contain antiseptics is also an advantage in terms of sustainability and resistance development.
Piezo technology
Technological developments have also improved ultrasonic scaling and mechanical depuration techniques. NSK has Intelligent Piezo, an ultrasonic scaler that can distinguish between calculus and the root surface. This ensures that only calculus and biofilm are removed, while the root surface is preserved. The treatment is fast, efficient and more comfortable for the patient.
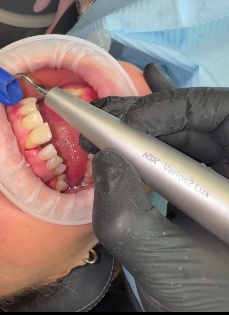
Hand instruments are still important but are increasingly used as a supplement to control the work of the ultrasonic scaler.
Ultrasonic scaling creates a cavitation effect that breaks down the biofilm and eliminates bacteria, as well as acoustic streaming that removes dissolved particles from the pockets.
NSK offers a wide range of more than 80 different tips suitable for use with the Varios Combi Pro2 for minimally invasive treatment. Find out more here.

Efficiency and patient comfort
Modern, minimally invasive equipment is not only gentle, but also efficient and timesaving. Clinicians are exposed to less strain, while the patient experiences a faster and more comfortable treatment.
To view more NSK content for dental therapists and dental hygienists, visit mynsk.co.uk/ikigai.
References
- World (2025). New data: noncommunicable diseases cause 1.8 million avoidable deaths and cost US$ 514 billion every year, reveals new WHO/Europe report. https://www.who.int/europe/news/item/27-06-2025-new-data–noncommunicable-diseases-cause-1-8-million-avoidable-deaths-and-cost-us-514-billion-USD-every-year–reveals-new-who-europe-report
- How does ultrasonic cavitation remove dental bacterial biofilm? Vyas N, Wang QX, Manmi KA, Sammons RL, Kuehne SA, Walmsley AD. Ultrason Sonochem. 2020 Oct;67:105112. doi: 10.1016/j.ultsonch.2020.105112. Epub 2020 Mar 28.PMID: 32283494 https://pubmed.ncbi.nlm.nih.gov/32283494/
This article is sponsored by NSK.

