
Justin Durham and Alexandra Penn discuss the rise of mobile health and how adopting it could help dental professionals support patients after they leave the chair.
Dentistry has always been an early adopter of digital innovation. From CAD/CAM systems and automated laboratory workflows to digital radiography and intraoral scanners, dentistry has consistently embraced technologies that improve precision and efficiency.
The focus of these innovations has remained largely consistent: optimising the clinician experience. Digital tools have been used to streamline workflows, augment diagnostics, increase patient throughput, and improve access to services such as online booking and communication. In some cases, they have also improved patient comfort, for example, intraoral scanners, which have become a clear point of difference for practices, particularly for patients with a strong gag reflex.
At the same time, patient expectations are evolving. Increasingly, patients are not only choosing providers based on in-practice experience, but also on their ability to offer ongoing support, accessibility and continuity of care between visits.
Despite this shift, most digital innovation in dentistry has focused on what happens within the practice. As a result, one area remains comparatively underdeveloped: supporting patients after they leave the chair.
The efficiency era of digital dentistry
Up to now, digital dentistry has focused on improving efficiency and delivery of care within the clinic. Even more recent innovations, such as artificial intelligence (AI), have had a similar focus.
AI is increasingly being used in note-taking, radiographic diagnostics, treatment planning, and patient communication systems. These tools can improve consistency, support practice management, and in some cases enhance decision-making.
However, their primary impact remains within the clinic – continuing the trend of supporting clinicians, rather than fundamentally changing how patients engage with their care and clinician over time.
The reality of oral health: it happens outside the clinic
In wider healthcare, mobile health (mHealth, a form of digital healthcare) has transformed how patients engage with their conditions. From diabetes management to mental health support, digital tools now play a central role in helping patients manage their health between appointments.
Dentistry, by contrast, has been slower to adopt this shift.
Like many areas of healthcare, oral health outcomes are heavily influenced by patient behaviour. Prevention, symptom management and long-term outcomes rely on patients:
- Understanding their condition
- Adhering to advice
- Maintaining consistent routines
- Recognising changes in symptoms.
In other words, much of oral healthcare happens in daily life – not only during appointments.
The gap in the current model of care
Dental care remains largely episodic, delivered within time-limited appointments. Sometimes these appointments now have sizeable periods between them due to robust evidence on risk-based recall intervals.
Yet many conditions require ongoing self-management especially those living with persistent or recurrent conditions. Clinicians provide high-quality self-management advice, but its effectiveness can depend on what happens afterwards and therefore between appointments.
Without structure, reinforcement, or ongoing support, even well-delivered guidance can be inconsistently applied between appointments. Patients leave with good intentions, but understandably may forget key advice, struggle to implement essential habits, and may not fully recognise that looking after oral health is fundamental to overall health.
This is not a failure of patients or clinicians, but a limitation of the current model of care.
Dentistry’s slower adoption with signs of change
Bar a few exceptions, dentistry has been slower to adopt mHealth approaches. An example of adoption that enhances patient engagement while maintaining clinical oversight comes from orthodontics where some systems allow patients to upload photographs of their clear aligner progress, enabling clinicians to monitor treatment remotely and intervene when needed.
However, these examples remain relatively isolated. The broader opportunity, using digital tools to support patients between appointments, remains largely untapped within dentistry.
Why this matters for clinics
As patient expectations evolve, digital capability is no longer just about internal efficiency, it is becoming a point of differentiation in how care is delivered.
Patients increasingly expect not only high-quality treatment, but also ongoing support and continuity between visits. Practices that can provide this are likely to be perceived as more modern, more supportive and more aligned with wider healthcare trends.
Supporting patients between appointments does not necessarily demand increased chair time or clinician workload. Digital tools can be used to extend care outside of appointments in a structured way – reinforcing advice, supporting adherence, and improving patient engagement without adding pressure to already busy clinics.
JawSpace: applying mHealth to TMD self-management
Temporomandibular disorders (TMD), a group of painful musculoskeletal conditions affecting the jaw joint and masticatory muscles, impacting approximately one in 15 people, provide a clear example of where mHealth can add meaningful value.
Self-management is accepted worldwide as the foundation of all initial TMD care, as it helps most patients control their symptoms using six core pillars (Figure 1).
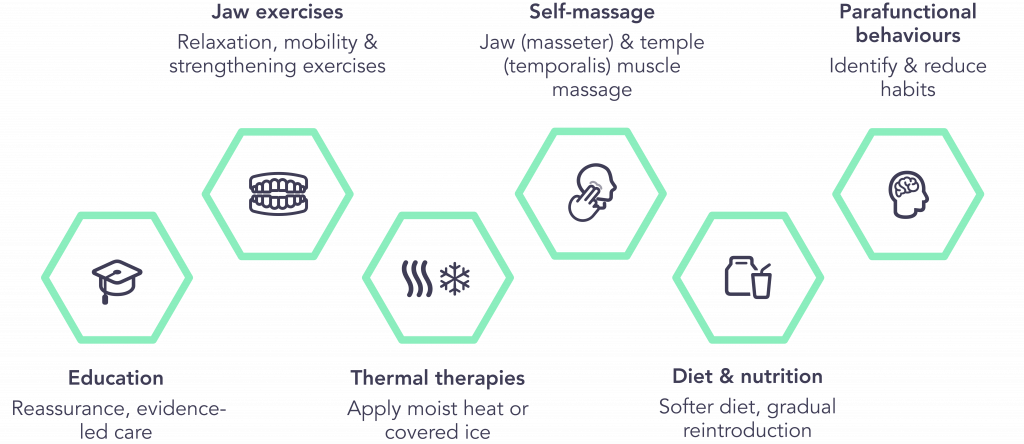
However, in practice, self-management is often delivered through verbal instruction, sometimes supported by written materials, with limited reinforcement beyond the appointment. As a result, adherence can vary, and key advice may not be consistently applied.
Digital tools offer an opportunity to address this gap.
JawSpace has been developed as a Software as a Medical Device (SaMD)* to support self-management in patients with a diagnosed TMD. It provides on-demand access to evidence-based information, alongside tools that support consistency and engagement between appointments.
For example, symptom tracking allows patients to recognise patterns and monitor progress, while prompts and reminders support adherence to recommended exercises and behavioural strategies. Structured reporting can also help reduce recall bias during review appointments, supporting more informed clinical discussions (Figure 2).
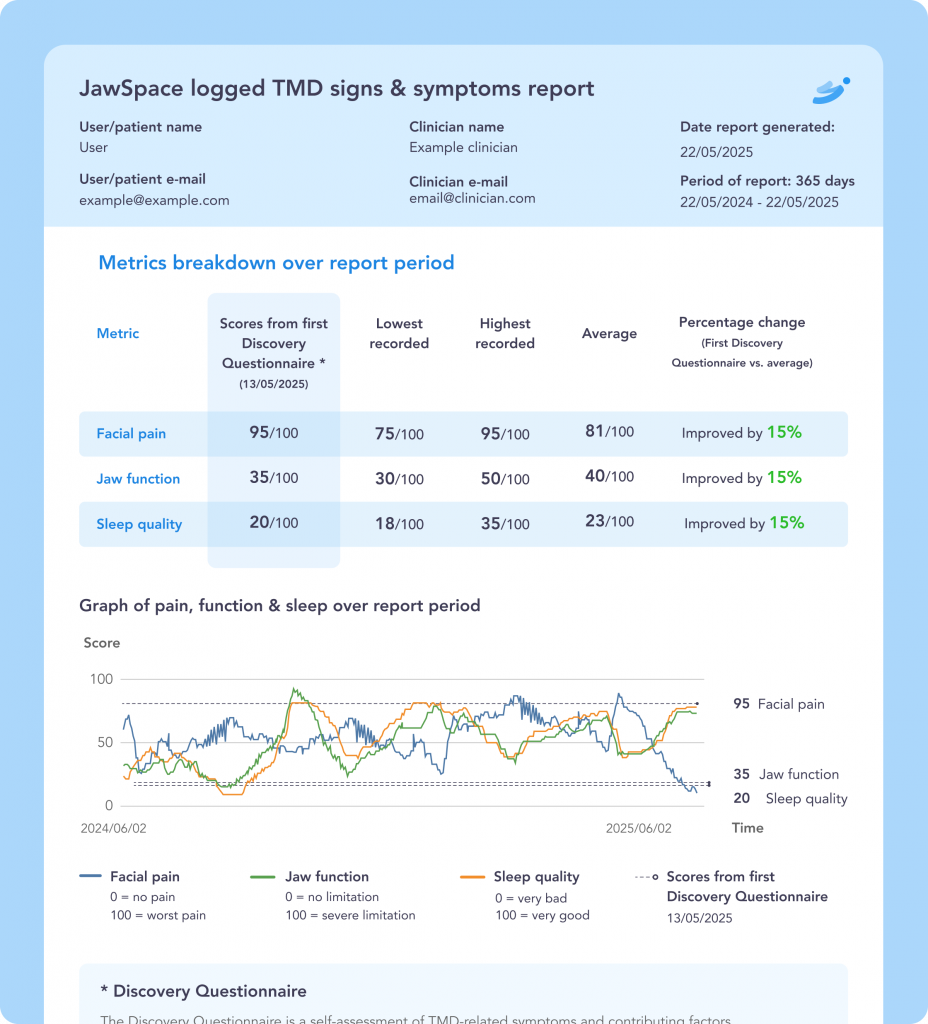
Importantly, tools such as JawSpace are at their best when integrated into the clinical pathway – introduced and supported by the clinician and aligned with in-chair advice.
Rather than replacing clinical care, this approach reinforces the clinician’s role, extending support beyond the appointment and helping patients engage more consistently with self-management.
Looking ahead
Digital dentistry has already transformed how care is delivered within the clinic. The next phase of innovation will focus on what happens beyond it.
As patient expectations evolve, and as prevention becomes a central focus of care, there is a growing need for tools that support patients in their daily lives – not just during appointments.
For dentistry, the question is no longer whether digital technology has a role to play. It is whether we are using it to its full potential.
Learn more about integrating TMD self-management and JawSpace into your clinical care.
Clinicians can try JawSpace complimentary for one month.
*JawSpace is a Class I Software as a medical device registered on the MHRA. It does not diagnose, treat, or replace consultation with a qualified healthcare professional.
Reference
- Durham J et al Self-management programmes in temporomandibular disorders: results from an international Delphi process. J Oral Rehabil. 2016 Dec;43(12):929-936.
This article is sponsored by JawSpace.

