
Lisa Knowles and Kate Reading discuss how they are expanding dental hygiene appointments through lifestyle medicine.
Imagine if one of the most effective ways to prevent chronic disease was not found in the GP surgery, but in the dental chair. Dental hygiene appointments, while traditionally focused on oral health and early disease detection, can serve as an entry point for broader preventive care. Dental hygienists and dental therapists are preventive healthcare professionals with the potential to impact more than just oral health.
By broadening our focus beyond biofilm removal to also incorporate lifestyle medicine principles, we can transform hygiene appointments into key opportunities for whole-person preventive care.
Providing practical lifestyle advice alongside comprehensive periodontal treatment positions us to help patients prevent illness, reduce oral disease, and coordinate care that bridges dentistry and the greater healthcare system.
Embracing lifestyle medicine in dental hygiene
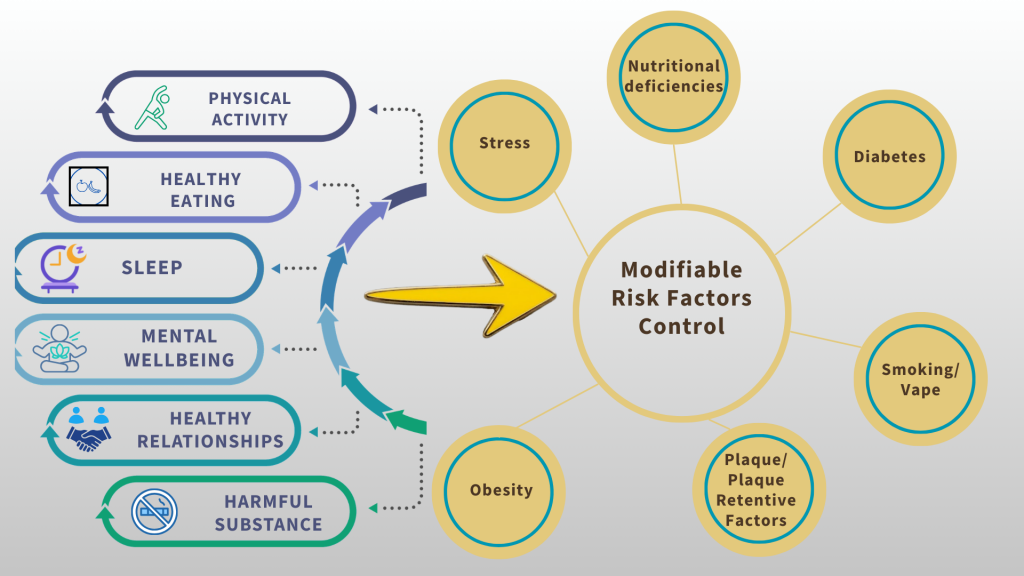
Based on six key pillars, lifestyle medicine embraces a whole-person approach to health. This framework recognises nutrition, physical activity, restorative sleep, stress management, social connection, and minimising harmful substances as essential to overall wellbeing, helping to reduce or even reverse chronic illness.

Oral health significantly influences overall disease risk. By adopting an evidence-based lifestyle medicine approach and providing advice on shared risk factors, without making diagnoses, we broaden our professional role.
According to the British Society of Lifestyle Medicine, this approach creates comprehensive, person-centred appointments and fosters meaningful discussions with patients.
Align with a broader, global movement
Noncommunicable diseases (NCDs) cause more than 43 million deaths each year, with oral diseases affecting nearly 3.5 billion people; more than the other main NCDs combined (World Health Organization, 2025).
The World Health Organization’s 2022 status report advocates a six-by-six framework that includes oral health and sugar intake in NCD prevention. This highlights the vital role of dental professionals in discussing these issues and collaborating with other medical disciplines to enhance preventive care (Jain et al, 2023).
Periodontal disease is an inflammatory condition connected to chronic illnesses. Addressing oral inflammation and key risk factors, like tobacco use, alcohol, diet and stress, not only improves oral outcomes but also systemic health.
Using lifestyle medicine principles during our appointments gives us a structured, confident approach to managing more sensitive issues such as smoking, diabetes, obesity and stress (Oh and Yu, 2021).
Redefining the hygiene appointment
As dental hygienists and therapists, we see how much broader health issues pass through the hygiene chair. We often see patients more frequently than other healthcare workers, sometimes before they notice health issues, which has changed our view on routine care visits.
Hygiene appointments go beyond plaque removal, serving as a gateway to overall health due to the link between periodontal disease and systemic conditions like cardiovascular disease, diabetes, and pregnancy issues (Tattar, Dias and Neves, 2025).
Each time we link oral symptoms to wider health, we’re reminded that prevention is at the core of our role.
Lifestyle medicine provides us with a common language and framework for what we already practise: supporting nutrition, physical activity, sleep, stress management, avoiding harmful substances and promoting social connection are central to patient-centred care.
From lifestyle clues to clinical insight
Lifestyle indicators often manifest in oral health before they are documented in medical records. High sugar intake, smoking, vaping, poor sleep, chronic stress and regular alcohol consumption all speak through plaque, bleeding and inflammation, which we now recognise as markers not only of local disease but of wider inflammatory burden (Sanz et al, 2020).
In this context, periodontal assessment becomes inflammation assessment; dietary discussion evolves into a metabolic health conversation; smoking cessation broadens into behavioural risk reduction; and stress management naturally links to bruxism, immune function and chronic disease risk (Public Health England, 2014).
Rather than feeling like ‘scope creep’, this feels like scope fulfilment, and sits comfortably within UK prevention guidance and periodontal care pathways (Oral Health Foundation (2026).
Putting lifestyle medicine into practice
Our method began by adding a lifestyle screening assessment to our appointments, in addition to our usual data collection, including a systematic evaluation of sleep, stress, physical activity and nutrition within the lifestyle medicine domains.
These insights help us build a richer picture and have more meaningful, measurable conversations. We’ve found that a curious, non-critical tone encourages patients to share more, supporting research that patient‑centred communication improves oral health behaviour (Gillam and Yusuf, 2019).
Asking patients what matters most to them or which habit most affects their gum health encourages open, honest discussion (Gillam and Yusuf, 2019). Each visit, we focus on one achievable change, like better sleep or consuming less sugar, to make progress manageable and realistic, therefore increasing motivation.
We developed Periolife Align after becoming colleagues at a Wilmslow referral practice and earning a certificate in lifestyle medicine coaching. The social media platform aims to integrate these principles into daily clinical practice, promoting collaborative, lifestyle-focused discussions as an essential part of periodontal care.
It helps educate patients on the relationship between chronic conditions – such as diabetes, obesity and cardiovascular disease – and oral health, using evidence-based lifestyle medicine principles.
With thanks to our sponsor, NSK.
References
- World Health Organization (2025) Noncommunicable diseases
- N, Dutt U, Radenkov I, Jain S (2023) WHO’s global oral health status report 2022: Actions, discussion, & implementation. Oral Diseases 30(2)
- Oh TJ, Yu SH (2021) Treatment of stage I-III periodontitis. The EFP S3 level clinical practice guideline. J Evid Base Dent Pract 21(4): 101638
- Tattar R, Dias B, Neves VCM (2025) The interrelationship between periodontal disease and systemic health. Brit Dent J 239(2): 103-8
- Sanz M, Del Castillo AM, Jepsen S, Gonzalez-Juanatey JR, D’Aiuto F, Bouchard P, et al (2020) Periodontitis and cardiovascular diseases. Consensus Report. Global Heart 15(1): 1
- Public Health England (2014) Smokefree and smiling. Helping dental patients to quit tobacco (second edition)
- Oral Health Foundation (2026) Delivering Better Oral Health: An Evidence-Based Toolkit for Prevention (version 4)
- Gillam DG, Yusuf H (2019) Brief motivational interviewing in dental practice. Dent J (Basel) 7(2): 51
Follow Dentistry.co.uk on Instagram to keep up with all the latest dental news and trends.

